If at first you don’t succeed… An expert’s guide to revision hip replacement
Autore:Our hips are essential for our ability to walk. If something happens this joint, the impact on our lives is huge. For this reason, many patients opt for hip replacement procedures, which install a prosthetic joint. However, sometimes this is not the end of the problem. We asked accomplished orthopaedic surgeon Mr Julian Gilbody why some patients need a revision hip replacement and what causes their first procedure to fail.
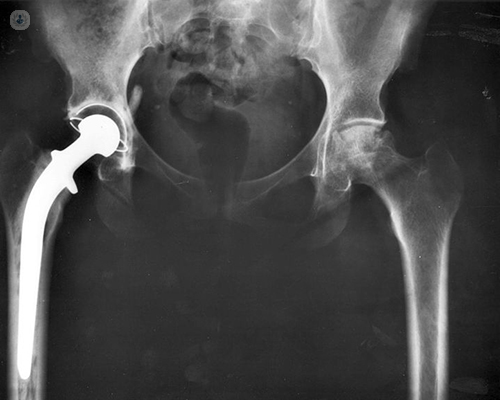
How long does a replacement hip last?
The best data we have on the longevity (or 'survivorship') of hip replacements comes from the National Joint Registry. This was started in 2003 and currently, every joint replacement done in England and Wales is included. The most recent annual report was published in September 2018 and contains data on 992,090 hip replacements. Looking at all hip replacements, the failure rate is about 0.5% per year, or to put it another way, after 10 years, around 5 out of every 200 people with a hip replacement will have had it revised at some point.
That being said, there are some factors which may make hip replacements fail sooner, or help them survive longer. It tends to be the case that the younger a patient is when they have their hip replacement, the quicker it will wear out - presumably due to increased activity levels, which increase wear rates. In contrast, some aspects of hip replacement design may reduce wear rates, such as using a ceramic bearing rather than a metal one.
What causes a hip replacement to fail?
There are different modes of failure for hip replacements. In the first couple of years after the operation, the most common reasons for revising a hip replacement are recurrent dislocation (where the ball keeps slipping out of the socket) and infection.
The infection rate is very low - around 7 cases in every 1,000 - but the problem here is that if bacteria get into the joint, they can adhere to the surface of the implant, and then often the only way to eradicate the infection is to remove the implants and re-do the hip replacement.
As time goes on, failure due to loosening and wear predominates, and this is still the most common cause for revision surgery. As with any mechanical system, the more the joint is used the more worn it becomes. Wear debris accumulates in the joint and can cause loosening between the implant and the bone. This usually takes several years for 'traditional' metal-on-plastic hip replacements (i.e. where a metal ball articulates with a plastic socket). It can be accelerated in certain types of metal-on-metal hip replacements.
Other causes of revision hip replacement surgery include peri-prosthetic fracture (a fracture which occurs around one of the implants), malalignment (incorrect positioning of the implants) and implant fracture (breakage of the actual implant).
How do you know when you need a second hip replacement surgery?
This depends on why the hip is failing. If it is due to recurrent dislocation, the problem is obvious.
Infection is usually obvious if there is pus discharging from the wound, but this is not always the case. Hip replacements can become infected with organisms which are of low virulence (i.e. they wouldn't normally cause an infection and can only do so because of the presence of foreign material) and may take many months to cause symptoms, which may be something as subtle as pain. A hip replacement which becomes painful several months after surgery should be investigated for possible infection. Furthermore, hip replacements can become infected many years after surgery by blood-borne infections that have arrived from another part of the body, e.g. skin infections. Fortunately, this is quite rare.
An implant which is affected by wear may manifest as dislocation which occurs several years after surgery, or less dramatically, there may be a sensation of the joint 'giving way.' Loosening may be experienced as pain, either in the groin or buttock area (if the cup is loose) or in the thigh (if the stem is loose). Some people may have evidence of loosening on X-rays, but if they are not experiencing any symptoms from the hip (pain/ giving way), it may not require revision surgery.
How long does it take to recover from a hip revision?
This is difficult to predict because it depends a great deal on how much damage was done to the joint before surgery, and how fit the patient is. Someone who is experiencing giving way because of wear, but whose implants are not loose, and who is generally fit and well, may recover almost as quickly from a revision operation as someone who is having it for the first time. On the other hand, a patient who has become very frail and who has also lost a lot of bone around the hip from loosening, requiring extensive reconstruction, may never return to their previous level of activity.
It is particularly important that as far as possible, any other medical issues are optimised before surgery to ensure the best possible outcome, and that the surgery is done in a unit that is able to look after all the patient's care needs and provides a good post-operative rehabilitation service.


