Aortic aneurysm in the abdomen
Written by:Our blood vessels are very important, carrying blood, oxygen, and nutrients around our bodies to keep us alive. Therefore weak spots on the blood vessel walls known as aneurysms can be a serious problem. But what exactly is an aortic aneurysm? What happens when you have one in your abdomen? Expert Mr Barun Majumder explains:

What is an aortic aneurysm?
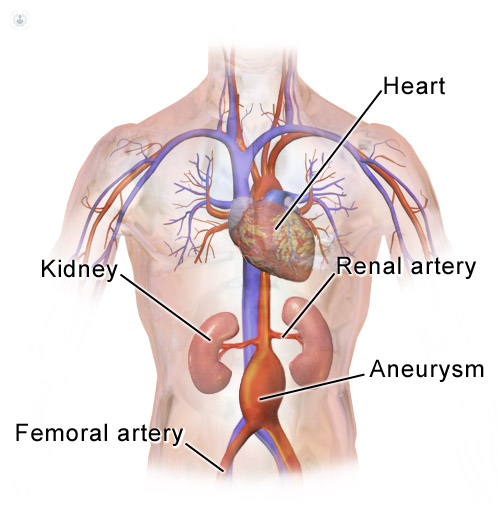
An aortic aneurysm is a bulge or ballooning of the artery, which starts in your chest, moving down into the abdomen and then into your pelvis and legs. It occurs due to weakness in the wall of the artery. There are several risk factors for this swelling of the artery, including:
- Smoking
- A family history of aneurysm
- High blood pressure
- High cholesterol
- Diabetes
Can you survive an abdominal aortic aneurysm?
Yes, there is a better chance of survival when the aneurysm is detected before it reaches 5.5 cm in diameter, i.e. with screening programmes. Aneurysms are also often found by chance during a scan for other symptoms. An elective planned repair of the aneurysm is best chance of survival. However, if it ruptures, the chances of survival are grave – it is fatal in 80% of cases.
What are the symptoms of a leaking abdominal aortic aneurysm?
The signs of a leaking abdominal aortic aneurysm are:
- Sudden, severe pain in the abdomen or lower back
- Cold, clammy extremities
- Low blood pressure
- Fainting or loss of consciousness
Frequently, in a slightly more stable patient, the symptoms may mimic a perforated ulcer, kidney stone, pancreatitis, or acute abdominal pain from other causes.
Diagnosis of a ruptured aneurysm is often established by an ultrasound in the A&E or by a CT scan in a relatively stable patient.
However, the condition may go unnoticed – sometimes diagnosis is only made during surgery, while in some cases it may not be discovered until after death during a post-mortem examination.
How big does an abdominal aortic aneurysm have to be to operate?
Normally, the main artery in your body measures between 1.5-3 cm and if it is larger than 3 cm we establish a diagnosis of aneurysm. Most aneurysms occur in the abdomen, and it is common in men over 65 years of age. The aneurysm grows slowly – usually by 1-2 mm per year. However, its growth could be erratic, and the aneurysm must be monitored. Treatment is offered when it reaches 5.5 cm for abdominal aneurysms. This is based on evidence from a randomised control trial, which proves that risks involved in surgery are greater than the risk of rupture below 5.5 cm. However, the risk of rupture outgrows the risks of surgery after 5.5 cm.
There is a national screening programme, which started in the UK in 2009 offering screening of males over 65.
Sometimes we offer surgery to patients with an aneurysm below 5.5 cm in the following circumstances:
- You are suffering from pain and your aneurysm is tender to the touch due to unusual rapid increase in size
- During the aneurysm surveillance programme, ultrasound shows the growth/increase in size of the aneurysm is more than 0.5 cm in 6 months or more than 1 cm in a year.
If you are concerned that you may have an aortic aneurysm, you should consult your doctor or a specialist.


