Complex trauma treatment: what to expect
Written by:Once a complex trauma injury has been assessed, it will need to be treated. Surgery may not always be required, but sometimes it is the only option. Highly experienced consultant orthopaedic surgeon Professor Mohamed Imam enlightens us on what to expect for complex trauma treatment in this final article of his complex trauma series.

How are they treated typically? What is the most effective form of treatment?
The priorities in orthopaedics are obvious; first, save the life then save a limb. Orthopaedic injuries in patients with polytrauma present unique diagnostic and therapeutic challenges. Multiply injured patients can follow numerous, often unpredictable, clinical trajectories and continuous re-evaluation of the patient’s physiology is critical to guiding treatment. The evaluation and treatment of multiply injured patients requires a coordinated, multidisciplinary approach. Patients with multiple-system injury and unstable fractures are managed best in a collaborative fashion.
How are complex trauma fractures treated?
The management of fractures has improved considerably with excellent outcomes over the last few decades. These excellent outcomes can be obtained through early intervention by staying relatively active whilst keeping the fractured segment immobilised and subsequent rehabilitation to increase strength and range of motion. Bespoke rehabilitation for each fracture based on patient and fracture characteristics are crucial for optimising the outcomes and to restore previous pre-injury levels. A collaborative multidisciplinary team (MDT) approach led by surgeons, anaesthetists, physiotherapist, occupational therapists, pain specialists, and patients themselves will ultimately lead to return to pre-injury activities of daily living, leisure, sport, and work.
A surgeon decides how to treat a fracture based on a number of factors. These include:
• age
• medical history
• type of fracture
• surgical expertise
The main goal in treating a fracture is to reduce the amount of pain patients are having in while giving you as much mobility as possible and allow to resume full range of motion and activity to pre-injury level.
What are the different treatment options for complex fractures?
There are two categories of treatment options.
Bracing or casting
Once bones have been repositioned, a cast made of plastic or fibreglass can be placed over the injured area. A brace works the same as a cast but allowing more mobility in nearby joints. This can't be used in all fractures, especially more severe ones.
Pins, screws, and plates
This type of treatment requires an operation. First, the bones and fragments are repositioned and realigned. Pins, screws, and/or metal plates are then inserted in a fashion to help hold bones in place during healing.
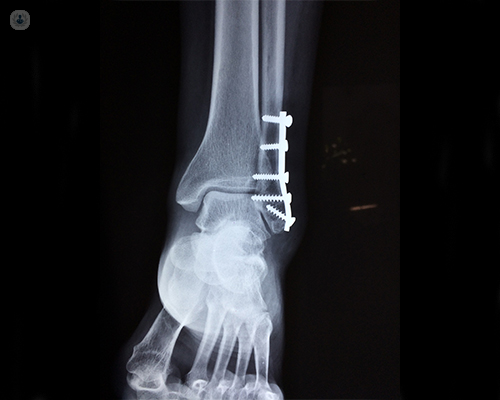
May surgery be required to heal these complex injuries?
The ultimate target is to enable patients to return to their pre-injury levels. Surgery might be the only option in many of the complex trauma presentations. All these patients should be managed in a collaborative manner. Better understanding and identification of these injuries enables us to optimise the outcomes. There are some fractures where surgery is the only option. Surgery is usually the only treatment option for a hip fracture, fractures that involve the joint surface, proximal scaphoid fractures, and fractures that compress on the nerves. Injuries that are associated with vascular injuries or dislocated joints require surgery.
Orthopaedic injuries place the patient at risk for various complications, including fat embolism, pneumonia, deep vein thrombosis, and sepsis. Many studies have documented the benefits of early stabilization in reducing morbidity and mortality. Early definitive long bone fixation and external fixation methods have evolved and are considered an integral part of the initial care.
Innovative techniques like computer-assisted surgery continues to develop as technology improves. Uses in trauma include navigation for percutaneous screw placement in trauma surgery and for replacement surgery for reconstruction of complex fractures. Additionally, computers may provide assistance with starting points for interlocking screws, intramedullary nailing, and rotational reduction.
Creating models of complex fractures via three-dimensional printing can aid in pre-operative planning. A complex deformity corrections simulation can be virtually performed before surgery.
Minimally invasive surgical techniques are used to achieve fracture reduction and stability with minimal soft-tissue disruption throughout the body. Minimising the disruption of critical soft-tissue attachments in the fracture zone, which are frequently disrupted or cleared using traditional approaches, is the main benefit of these approaches.
Specialised implants have been developed for the proximal humerus, allowing minimally invasive insertion and optimal stabilisation for metaphysical fractures in the upper extremity. Diaphyseal fractures of the upper and lower extremity can be managed with minimally invasive techniques using non-specialised hardware. Implants that optimise stabilisation of the dismal femur, proximal tibia, and distal tibia in the lower extremity continue to be optimised.
Biologic adjuvants improve fracture healing by providing biologic media that would augment the environment for fracture healing. Examples of biologic adjuvants include bone graft, bone substitutes, platelet-rich plasma, autogenous bone marrow, calcium combinations, parathyroid hormone, bone morphogenetic protein, and stem cells. Although a useful tool, biologic adjuvants are not a substitute for a well-thought-out preoperative plan and surgical execution, but can aid the overall treatment strategy.
If you recently experienced complex trauma and would like to schedule a consultation with Professor Imam, you can go to his Top Doctors profile and book a visit.


