Gout attacks and management tips
Written by:Gout is caused by excess uric acid in your body and the condition is actually a form of arthritis. Dr Gerald Coakley, a leading rheumatologist, explains how this occurs, the symptoms, how food and drink habits affect attacks and he provides tips for managing this condition.
What is gout?
Gout is a disease in which crystals form in the joints, and sometimes in the soft tissues. It is caused by an excess of uric acid and this acid is produced during the breakdown of purines, (natural compounds), two-thirds of which are made naturally within our bodies and one third is derived from protein that we consume from our diet. People with gout have a reduced ability to flush out uric acid properly through urine. When it builds up to a critical level, it forms uric acid crystals which are extremely irritating to a joint.
Gout attack: how long does it last?
Gout attacks typically last for a few days or up to a week. In serious long-term cases, attacks can go on for weeks or even months continuously.
What are the symptoms of gout?
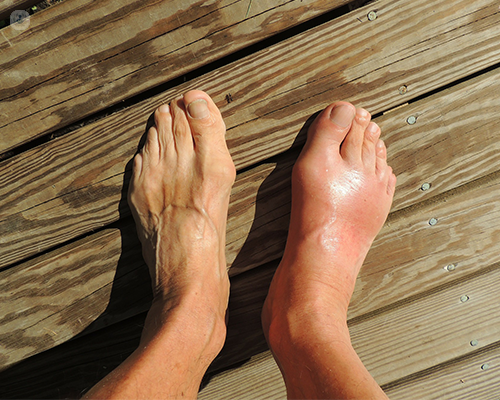
Almost always, gout starts in either a big toe joint or an ankle. The affected joint becomes intensely painful, red, hot and swollen. Furthermore, the skin over the joint may appear shiny and may peel. The pain increases to a peak within 24 hours and can be so severe that even contact with a sock or bedsheet becomes unbearable.
Over the decades, without effective treatment, it ascends up the body to the knees and then later to the hands and elbows. At the later stages, uric acid builds up in the soft tissues around joints, forming hard lumps known as gouty tophi. These are made of pure liquid uric acid, and in some cases, the tophi will discharge through the skin – it looks golden-yellow, like Jersey cream.
How do food and dietary choices affect gout attacks?
While people who don’t drink alcohol do get gout, the most important cause of gout in Western countries is excessive consumption of beer, especially lager. It is important, if you suffer from gout, to not exceed government guidelines on the safe intake of alcohol. This means no more than 14 units of alcohol per week, which is seven pints of beer or one and a half bottles of wine per week. If you are a regular beer drinker, many rheumatologists would recommend a switch to wine.
It makes sense if you suffer from gout to reduce foods that are high in proteins. This means red meat, particularly offal like kidneys or liver, as well as oily fish like mackerel and sardines, and yeast extract foods like Marmite or Bovril. Less purine-rich foods include beans, pulses and poultry.
There is a strong link between being overweight, having a high cholesterol level, type-2 diabetes and gout. Therefore, one of the most important lifestyle measures we recommend for anyone with gout is to reduce weight if you are overweight.
What tips can you share for managing living with the condition?
Drinking plenty of water can reduce the risk of gout attacks. You should aim to drink at least one litre of water per day and up to 3.5 litres per day if you have kidney stones. Try to avoid sugary soft drinks because they contain a lot of fructose which increases the uric acid level in the blood.
Gout is quite a common type of arthritis that, from the perspective of a rheumatologist, is very rewarding to treat. That is because, with the correct management (usually with either Allopurinol or Febuxostat), it is possible to reduce uric acid levels to normal and stop any further attacks of this extremely painful form of arthritis. There are few similarly treatable conditions in medicine.
However, it is often not very well managed because traditional medical teaching for the management of gout has not been based on the best evidence, and many non-specialists choose the wrong treatment for the wrong duration of time.
The most important thing if you are having trouble with your gout is to seek the opinion of a rheumatologist. They can confirm or rule out the diagnosis, and advise on the best treatment for your particular circumstances. Once the treatment is established and has brought the serum uric acid into the target range (the lower half of the normal range for serum uric acid), you will be able to manage the condition with the support of your general practitioner.
How long will I need treatment?
It’s important to understand that, once uric acid-lowering medication for gout is started, it must be taken for life. This may seem daunting, but the medication is generally extremely well-tolerated, completely prevents further painful attacks of gout and will protect your joints and kidneys from permanent damage by uric acid crystals.
View this online PDF from Versus Arthritis to learn even more about gout.
Click here to view Dr Gerald Coakley’s profile and learn how he can assist you with your health.


