How does haemodialysis (kidney dialysis) work?
Written by:
Haemodialysis is a lifesaving dialysis treatment for patients with chronic kidney disease (CKD), which has progressed to end stage renal disease (kidney failure). Dialysis replaces the functions that normal healthy kidneys would perform, such as cleaning the blood and removing excess urine. There are two types of dialysis; haemodialysis and peritoneal, but the following is about haemodialysis.
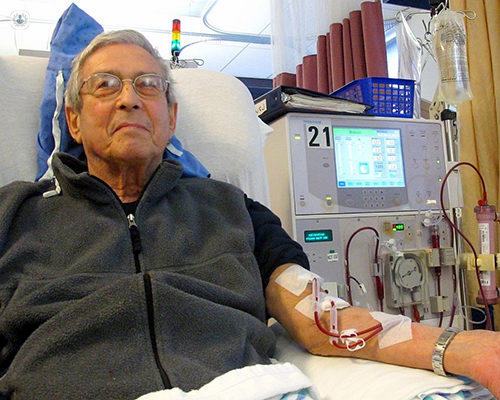
How does a haemodialysis machine work?
During haemodialysis a dialysis machine with a filter and an artificial kidney (haemodialyser) is used to clean the blood. To achieve access to the blood and to get blood into the dialyser, a minor surgery is performed using either a fistula, graft or a catheter.
Blood is removed from the body and circulated through a fluid circuit (outside of the body), where it is cleaned using dialysate and then returned to the patient. Dialysate is a washing fluid that helps remove the unwanted waste products from the blood and helps electrolytes and minerals to reach the correct level in the body. The machine also monitors the flow of blood and sometimes releases the sound of an alarm if something needs to be checked.
What waste products are removed by haemodialysis?
All waste products from the kidney will be removed such as those found in the blood. These include urea, creatinine, potassium and extra urine that pass through the membrane, which are washed away.
What are the risks of haemodialysis?
Haemodialysis is efficient in replacing some of the kidney’s lost functions but other conditions can be caused through the treatment, such as:
- Low blood pressure
- High blood pressure
- Anaemia
- Bone diseases
- Heart palpitations
- Fluid overload
How long does a haemodialysis procedure take?
It can take between three to four hours and is done three times a week. It can be done in a hospital or at home. If a patient decides to have the treatment at home, then the dialysis may happen four to seven times a week with shorter hours. The patient and doctor will determine the best place, depending on the medical condition of the patient.


