How it happens: inserting a dental implant
Written by:When there is a gap between your teeth, there are different options to fill the space. One option, and the most recommended option, is having a dental implant inserted. Professor Andrew Sidebottom, a highly-trained maxillofacial surgeon, provides information about what the procedure is, what is involved, and what to expect.
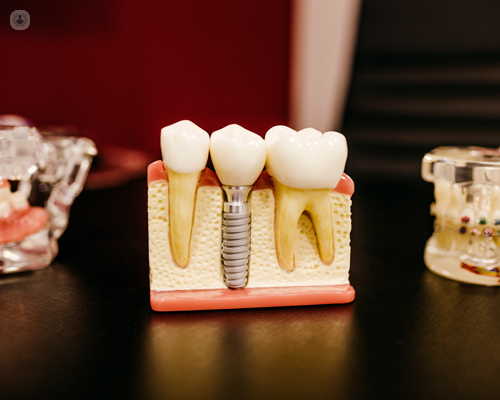
What is a dental implant?
A dental implant is a replacement for the root of a tooth typically made of titanium. Eventually, the bone and the implant should fuse together.
Your surgeon will assess if this surgery is the best option for you. This assessment may include photos and x-rays for medical records, and they may ask questions about medical history. The amount of bone available to fuse with the implant will also be assessed, and a CT scan or a model of your jawbone may be made.
Are there any alternatives to inserting a dental implant?
It is possible to leave the gap in your teeth, however, it may cause strain on your other teeth, gum disease, and issues with talking and eating.
Dentures, which are artificial teeth in removable plastic or metal frames, can be used to replace some (partial dentures) or all of the teeth (full dentures). Although, these are not appropriate for all people. Dentures may cause gums to recede and bone loss over time, as well as problems with talking and eating. They need to be removed for cleaning, and in due time they will need to be replaced after your mouth has changed and they have been worn down.
For a single-tooth gap, a bridge may be possible. The teeth on either side of the gap are cut down and an artificial tooth is attached to them with either cemented wings (bonded bridge) or with a crown (fixed bridge). This process results in significant damage to the teeth that are cut down to attach the bridge. It is a more reliable option than dentures and they do not move while talking or eating; however, bridges fail more than implants. If it’s even possible, a bridge might need to be replaced with a newer one, or possibly replaced with dentures or an implant. Some still require dental implants to support bridges and dentures.
What will happen if I decide not to have the operation?
The gap in your teeth will remain. Your existing dentures will continue to be loose if your doctor has recommended an implant to support them. A bridge or dentures may be an option with doctor assessment.
What does the operation involve?
Under local anaesthetic, some single dental implants may be inserted easily. Your doctor may offer a sedative or give general anaesthetic if the procedure will be difficult.
The procedure for each implant usually takes twenty minutes up to an hour, depending on the difficulty of the insertion and if a bone graft is needed.
A cut on your gum will be made, and a special drill will be used to create a hole in the jawbone. Then the implant will be screwed or tapped into the bone. If there is not enough bone, then a bone graft will be done. The doctor will take bone from the hip or lower jaw, or artificial bone may be used.
Either your gum will be closed over the implant or a metal stud to push through out of the gum will be left. If closed, it will usually be done with stitches and they may be dissolvable. You may be asked to bite on a pack of gauze for about ten minutes to stop any bleeding.
What can I do to help make the operation a success?
If you are a smoker, stopping smoking now reduces risk of complications, as well as improves your long-term health. Stopping smoking and keeping your mouth clean greatly cuts down the risk of infection and implant or bone graft failure.
Trying to maintain a healthy weight also reduces risk. If you are overweight, your risk of developing complications is higher. Before the operation, regular exercise should help to prepare. It should also help to recover and improve long-term health.
What complications can happen?
General complications that may arise:
- pain level related to difficulty of operation
- bleeding after the operation
- swelling and bruising; this is more common when a bone graft has been used
- infection; wound may take longer to heal and there is a higher risk of implant failure
Specific dental implant complications:
- Implant failure: 5 in 100 risk for non-smokers and 15 in 100 risk for smokers. Another implant or alternative may be assessed.
- Sinus problems: an opening in the sinus and the mouth may happen from inserting an implant into the upper jaw. Secondary problems may be infection (sinusitis), pain, fluid draining between the mouth and nose, and implant failure.
- Damage to neighbouring teeth: nearby teeth may become loosened and may need to be removed if they remain loose.
- Damage to nerves connecting lip and tongue: loss of feeling in lip or tongue may happen from inserting implant into the lower jaw. It is typically temporary, but can take up to eighteen months to recover.
What can be expected during recovery?
Once the bleeding has stopped, you should be able to return home the same day. Someone should take you home and stay for at least twenty-four hours if you have had a sedative.
If bleeding resumes at the site of the wound, press a pack of gauze or a clean handkerchief in a knot over the wound for ten minutes. Do not smoke and keep the mouth as clean as possible. Antibiotics may be given.
The wound should be left alone for one to two days. For the following two days, start gently rinsing the mouth with salt water four times a day. During at least a week after, rinse mouth with chlorhexidine mouthwash twice a day until brushing is comfortable again.
Avoid drinking alcohol, exercise, or hot baths for one week to reduce risk of bleeding, swelling, and bruising. Over-the-counter painkillers should help any discomfort and should be commenced immediately following the procedure.
Only soft foods should be eaten for one to two days and gradually moving to solid food when chewing is comfortable. Try using the other side of your mouth when chewing. Most people return to normal activities after two to three days following a single implant, but some people may need up to a week off work particularly if bone grafts are used.
If you are in need of a dental implant or would like a consultation to get more information, go to Professor Sidebottom's Top Doctors profile to schedule a visit.


