Neuroendocrine tumours (NETs): symptoms, diagnosis and treatment
Written by:Neuroendocrine tumours (NETs) are a rare type of tumour that can form in the neuroendocrine system. These may be in the gut, the lungs, or the pancreas. Symptoms differ depending on where the tumours form. Dr Christos Toumpankis, a leading gastroenterologist, explains what NETs are, the symptoms, how they are diagnosed and how they can be treated.
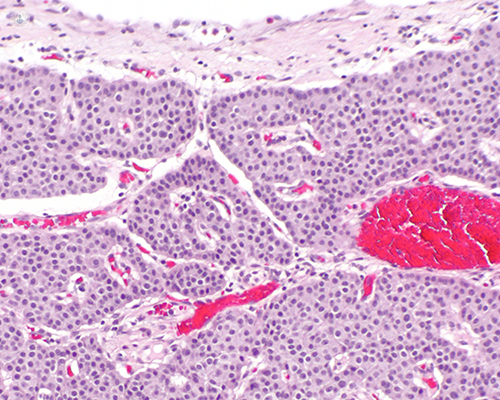
What are neuroendocrine tumours (NETs)?
Neuroendocrine tumours are a group of tumours that consist of specific cells called neuroendocrine cells, which can be found forming glands such as the pituitary, adrenal, and parathyroids, but also can be distributed in many organs, most commonly, the gut, the stomach, and the pancreas; this is where we find the majority of these tumours.
NETs have got five main characteristics:
- They are heterogeneous (they consist of different cells that play different roles).
- They are usually slow-growing.
- They usually secrete hormones and therefore can cause specific symptoms
- They may have receptors of somatostatin which is a specific hormone on their surface
- There is likely more than one treatment option.
In the past, NETs were considered rare, but that's not the case anymore. Recent studies have demonstrated that over the last 30 years, the incidence of those tumours has substantially increased, whereas the incidence of all other cancers has remained stable.
NETs can vary in how aggressive they are. If I can borrow the example of the old-fashioned Western “The Good the Bad and the Ugly” to divide them:
- “The Good” – slow-growing tumours, some of which may never spread
- “The Bad” – this group are tumours which are still slow-growing, but at some point, they'll spread
- “The Ugly” – this group are the tumours that become really aggressively and can look like other cancers.
The diagnosis of these tumours is based on a good examination of the patient’s medical history by the physician, a blood test and urine test, good quality imaging studies, and finally, on a biopsy.
What are the symptoms of neuroendocrine tumours (NETs)?
Symptoms of neuroendocrine tumours can be variable. Patients can present with:
- Chronic diarrhoea – diarrhoea for more than four weeks.
- Flushing – the face becomes red for a few minutes
- Chronic cramping pain
- Ulcers in the stomach or duodenum – these are difficult to treat
- Episodes of low blood sugar
Some patients have no symptoms. In those cases, neuroendocrine tumours can be revealed just incidentally.
How can neuroendocrine tumours (NETs) be diagnosed and are they ever misdiagnosed?
When making a diagnosis of neuroendocrine tumours, the physician should follow the steps of a history clinical examination, but also use high-quality imaging studies, such as the Gallium 68 PET scan, which is the most modern imaging modality that someone can use for NETs. This is a whole-body scan and can pick up tumours as small as 7 mm. Through that scan, tumours cannot be missed. However, tumours can be missed only if the physician does not suspect them.
How are neuroendocrine tumours (NETs) treated?
When we are treating a patient with neuroendocrine tumour, we're following four principles.
First of all, we are aiming to control the patient's symptoms and especially those which are related to hormonal secretion by the tumour. As soon as we achieve this, we discuss the patient case with our surgical colleagues to see whether they can resect the primary tumour or even the metastasis. If this is not possible, then we try to find ways to delay the tumour growth and even shrink the tumour. Last but not least, we, as physicians, try to improve and always maintain the patient's quality of life.
For the first target, control of the patient's symptoms, we are lucky to have easy medications (monthly hormonal injections) which can be given easily by the patient's GP, and some of them even by the patient themselves. Those injections can control the hormonal symptoms of the tumour, but also can delay tumour growth. If this is not possible, the physician who treats neuroendocrine tumours is lucky because he or she can choose from a variety of options, which can include:
- Chemotherapy
- Oral tablets
- Radiation treatment, both internal and external


