The advanced DEXA scan
Written by:There are many groups of people who are at risk of osteoporosis, and therefore there is quite a large range of potential people who may benefit from an advanced DEXA (dual-energy X-ray absorptiometry) scan.
This article explains all you need to know about the advanced DEXA scan, including what this diagnostic tool offers, how it differs from the standard DEXA scan, and what patients can expect after receiving their results.
What is a DEXA scan and what does it do?
A DEXA (dual-energy X-ray absorptiometry) scan is a machine that measures the apparent density of a patient’s bone. Its purpose is to diagnose osteoporosis and to identify the risk of fractures and bone breaks.
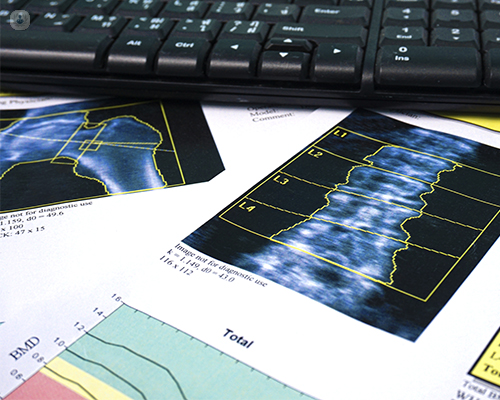
It uses two energies: a high energy beam and a low energy beam. The high energy beam will travel through the patient and the energy is collected by the detectors, whereas the low energy beam is absorbed by the soft tissues. Using these two energy beams, the machine detectors will produce measurements of bone and other density, and ultimately create a digitally-generated image of the bone.
The usual bones measured are the lumbar spine, found in the lower back, and the proximal femur, the upper part of the hips which many of us know as the hip joint.
Difference between advanced and regular DEXA scan
Unlike a standard DEXA scan, which only measures one hip, the advanced DEXA scan can measure both hips at the same time.
Furthermore, the advanced scan is used when necessary to view the spine from its side, offering a lateral picture. A lateral picture can allow a fracture or break in the lower spine to become identifiable, something which often shows no symptoms.
Furthermore, having recently become shorter or suffering from back pain might mean a patient has a collapsed bone - something which can also happen without back pain - and the advanced DEXA scan will be able to diagnose these fractures.
In addition to a standard (or basic) DEXA scan and the advanced DEXA scan, there is also a third type of DEXA scan called a body composition scan. This is used to analyse fat, muscle and bone. However, unlike the others, it cannot be used to diagnosis osteoporosis.
Who should have an advanced DEXA scan?
Anybody who is at risk of osteoporosis should consider a basic DEXA scan, but an advanced DEXA scan should be considered for all who know they have osteoporosis.
Although osteoporosis is usually considered in women over the age of 50 who are post-menopausal, there are many other groups at risk, including:
- Men and women over the age of 50.
- Men and women with eating disorders, as they are found to have low bone density.
- Women who are no longer menstruating, regardless of age. This could be due to early menopause or conditions such as eating disorders.
- Very athletic men and women.
- Anybody who breaks a bone while over the age of 50 - they could have a low trauma fracture.
- Patients who have been taking specific medications, such as steroid tablets.
- Women receiving breast cancer treatment - some drugs affect bone density.
- Women or men with a family history of osteoporosis.
- Anyone with rheumatoid arthritis (also known as chronic arthritis).
Those who would be especially suited to an advanced DEXA scan are:
- Men and women over the age of 50 who have noted height loss or acute back pain.
- Anybody over the age of 50 who has had a low trauma fracture.
- Patients who are on long-term steroid therapy.
- Women receiving breast cancer treatment.
- Older men on prostate cancer treatments.
- Women with a close family history of height loss or becoming bent over in later life.
How is an advanced DEXA scan performed?
Unlike with other scans and diagnostic procedures, the patient can eat and drink as normal before their appointment.
Before the scan, they will be asked to fill in a risk factor questionnaire. The answers are then entered into the scanner and after the measurement of the patient’s apparent bone density has been measured, the scanner will calculate a 10-year risk of the patient of suffering a major osteoporosis-related fracture as well as telling if they have osteoporosis.
Depending on the site being scanned, patients are usually required to take off some outer garments and will be asked to ensure they have no metal on any of their clothing. This metal could be in the form of trousers’ zips or clasps of bras. Any metal within the scanner field shows up on the image and disrupts the bone density results.
The patient will lie on the scanner and, depending on the site being analysed, they will lie in a specific position:
- Spinal scan - The patient lies on their back with their legs on a cushion so that the spine is flat on the table.
- Hip scan - The patient has to twist their hips and legs inwards with their hip bones flat on the table. To make this position easier to maintain, there is a positioning device which flattens the hip to allow a better view of the upper femur.
The scanning itself lasts around 5-10 minutes for each site. Depending on the number of sites being scanned, the entire appointment can take 20–30 minutes.
The radiographer and/or technician will evaluate the analysis from the machine to confirm it is reliable and then send the result to a doctor for a clinical report. It will then be sent to the referring doctor and patient.
Are the x-ray beams safe? What risks are associated with an advanced DEXA scan?
DEXA scans are very safe because the dose of radiation is extremely low.
To put this into perspective, any site being measured receives less than a third of the radiation you get from walking in the street every day. Having said this, it isn't recommended to have it frequently, usually no more than once per year.
Only a select few are highly advised against having an advanced DEXA scan:
- Pregnant women - even though the dose of radiation is extremely low, there is a risk that it could harm the foetus.
- Children - due to their young age, any radiation exposure, even if incredibly low, is advised against. However, if a child is on certain treatments, such as steroids, they might benefit from the scan despite the risk.
What course of action will a rheumatologist recommend after DEXA scan results?
If the results show that the apparent bone density is normal or a little less than average for the patient’s age group, they will likely be advised to adjust some lifestyle factors, including:
- Introduce weight-bearing exercises to their daily routine, such as walking, dancing, jogging or weight lifting, and generally any exercise that consists of going against gravity.
- Get sufficient vitamin D, acquired from diet or sunlight (summer sunlight), or if necessary, from a supplement.
- Consume adequate calcium.
If the results show that the patient has a high risk of fracture for their age, or if they do indeed have osteoporosis, the advice would be to start treatment in addition to lifestyle changes to tackle osteoporosis and combat bone loss. Approved treatments all reduce the risk of fracture.
In some cases, your rheumatologist will recommend a repeat scan in two or three years to check that the treatment is working.
If you’re worried about your own bone health or that of a loved one, don’t hesitate to book a consultation with an expert.


