Atrial flutter: your comprehensive guide
Written by:Atrial flutter is the sensation of rapid heartbeats and this eventually leads to a tired heart that requires urgent treatment. Read on to learn what this condition means for people with atrial flutter, it’s symptoms, how it’s treated and more, as explained by Dr Boon Lim.
What is atrial flutter?
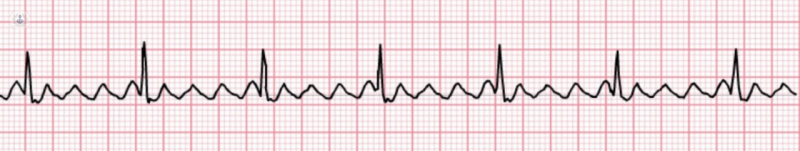
Atrial Flutter is a regular rapid rhythm of the atria (the upper chambers of the heart) which leads to a sensation of rapid heartbeats (palpitations). Readings from an electrocardiogram (ECG) show characteristic appearances that are diagnostic of the condition. The appearance of heart rate readings is a typical sawtooth pattern of conduction (image 1). Typically, the heart rates of atrial flutter are 150 beats per minute, but occasionally, particularly in patients over 70 years old, the rates may be slower. In atrial flutter, the heart rates are almost never consistently more than 150bpm.
How do you treat atrial flutter?
Atrial flutter is initially treated with drug therapy. Drugs that your doctor will consider include anticoagulation, commonly known as blood thinners, such as warfarin or a newer class of drugs termed ‘direct oral anticoagulants’ such as apixaban, rivaroxaban, dabigatran or edoxaban. In addition, if your heart rates are consistently elevated, your doctor may suggest a rate-limiting drug such as a beta-blocker (bisoprolol, metoprolol) or calcium blocker (verapamil, diltiazem).
While it’s initially treated with drug therapy, which may help minimise the risk of stroke and slow down the heart rate, this won’t cure atrial flutter. It’s ultimately cured by a catheter ablation strategy which has a very high success rate; around 95% of patients have no recurrence of atrial flutter after catheter ablation. In this procedure, catheters (flexible electrical tubes) are inserted through the groin via the femoral vein into the heart. Once it's in the right atrial chamber, radiofrequency energy is delivered to cauterize (burn) areas of the heart which are responsible for perpetuating this circuit that causes atrial flutter. The procedure takes anywhere from 45 to 90 minutes typically and can be done under local anaesthesia or general anaesthesia.
Why does atrial flutter need treatment?
Untreated atrial flutter will lead to a risk of progressive heart failure (weak heart muscle). Symptoms that may persist are:
- Shortness of breath
- Chest pain
- Tiredness
- Light-headedness
- Palpitations
This risk is particularly high if the heart rates in atrial flutter are left at a rate that is too high (i.e. consistently at 150bpm). Think of it as having to run a marathon but 24 hours a day – the heart never slows down to recover! At some stage, the heart may eventually become tired and fail to contract normally.
How are serious symptoms of atrial flutter immediately treated?
Serious symptoms (shortness of breath and chest pain) may need to be treated with emergency cardioversion. This is when electrical shock therapy is delivered to stop and restart the heart. However, this is likely to be a temporary solution as the flutter does persist and ultimately an ablation should be recommended to cure the condition. Drugs are also given immediately to reduce the heart rate and to minimise the risk of stroke.
When would ongoing medication be recommended?
In all cases of flutter, the initial strategy is to take medications. However, the ongoing use of medications will depend on whether a more permanent cure is performed (i.e. ablation). If ablation is done and the flutter no longer exists, then medications can be stopped. If ablation is not performed, then it is likely that medications will be continued in the long term.
When is ablation needed? Why aren’t all patients offered ablation?
Cardiac ablation for atrial flutter should be offered to most patients. However, in some cases, it’s difficult to offer a patient the procedure because:
- The patient is very frail
- They cannot lie down for an hour on the catheter lab table due to back problems
- The catheter lab cannot accommodate patients due to morbid obesity (weight >150kg)
Patient choice and education are very important and, in all instances, the full procedure should be explained to the patient (and relatives).
What are the success and complication rates of atrial flutter?
Atrial flutter ablation carries a success rate of around 95% with a minor complication rate (3%) of groin haematoma (bruising), and a very rare complication rate (less than 0.5%) of stroke, heart attack or cardiac perforation that would need emergency bypass surgery.
In more elderly patients with slow heart rates (typically 60 beats per minute or less) in atrial flutter, there is a risk of needing a pacemaker. This is not a complication but rather an indication that the electrical conducting system in the heart is not robust enough to sustain a normal heartbeat when this is restored.
Who performs atrial flutter ablation?
A cardiologist with a specialist skillset in ablation (electrophysiologist) performs ablation. These procedures are mainly carried out in larger specialised consultative cardiology units with the relevant expertise and support for electrical procedures.
If you would like to arrange to see a specialist electrophysiologist, please make an appointment with Dr Boon Lim via his profile.


