Facial paralysis: a guide to Bell's palsy
Written by:Facial paralysis can be a terrifying idea, but it is a very real condition that can prevent movement in half or even all of a person's face. But why does facial paralysis occur, and what causes it? Plastic surgeon and expert in facial paralysis Mr Paul Tulley answers these questions and more in this guide to all you need to know about Bell's palsy.
How does facial paralysis occur?
Facial palsy is paralysis of the muscles of facial expression due to damage or incomplete development of the facial nerve. This results in an inability to produce facial movements on the affected side of the face, such as smiling. Facial asymmetry may be present at rest.
More significantly, important functions such as eye closure may be affected, particularly in older patients, which can lead to secondary corneal damage and visual impairment if left untreated.
Facial paralysis on the affected side may be total or be present as an incomplete paresis.
The most common cause of acute facial paralysis is Bell’s Palsy, caused by a Herpes viral infection. However it may also be present at birth, as a congenital defect, affecting one or both (Moebius Syndrome) sides of the face. Other causes of the condition include trauma to the facial nerve, other types of localised infection or inflammation, or surgery such as excision of certain types of tumours in the cranial region. These most commonly include acoustic neuromas and parotid gland tumours.
What is Bell’s palsy?
Bell's palsy is the commonest cause of facial paralysis and affects people of all age groups. Men and women are equally affected. It is usually temporary. Symptoms generally start suddenly and have no obvious cause, often over a few hours or overnight. The main symptom is weakness or paralysis of one side of the face.
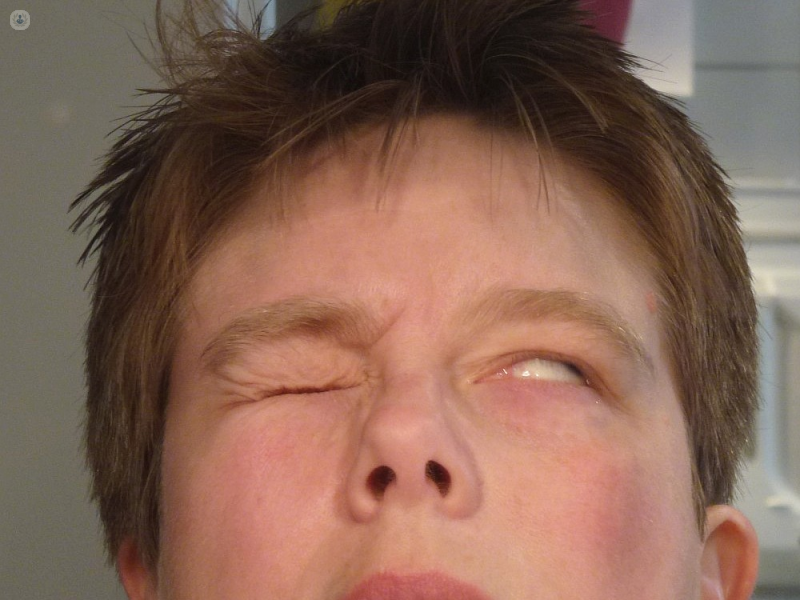
The eyebrow may also sag and eye closure is difficult. The eye can be dry or watery. Mild earache or pain behind the ear may be the first sign of Bell’s palsy in some patients. The mouth may droop and saliva and drinks can dribble from the mouth. Speech may be difficult and taste can be altered. Hearing is sometimes unusually sharp on the affected side of the face.
What causes Bell’s palsy?
Bell’s palsy is caused by herpes simplex virus infection of the facial nerve. The virus causes cold sores and is thought to lie dormant in the nerve root, causing swelling if it reactivates.
What is the best treatment for Bell’s palsy?
Bell’s palsy treatment includes using artificial tears to keep the eye moist and an eye pad or tape at night to keep the eye closed during sleep. Oral steroids may reduce the swelling of the nerve and prevent damage, particularly if they are commenced within three days of symptoms first starting. They are usually taken for 10 days. Antivirals (eg Valaciclovir) can be prescribed to treat the herpes virus, although there is little evidence that they help Bell's palsy. Facial exercises and physiotherapy may also be useful to aid recovery.
How long does it take to recover from Bell’s palsy?
Approximately 75% of patients with Bell's palsy recover completely spontaneously. Most patients have significant improvement within three to eight weeks of the start of the condition, but in others it can take three to six months before symptoms improve.
Around 15% of patients are left with residual facial weakness, muscle tightness or facial spasms. Spasm or facial tightness can be treated by botulinum injection to balance facial movement. Residual facial weakness and problems with eye closure can be treated with a range of surgical procedures such as facial slings, dynamic muscle transfers and eyelid surgery.



