Cervical cancer screening: what does it mean when CIN is detected?
Written by:Cervical cancer most commonly affects younger women, so it is important to have regular cervical smear tests to ensure that any sign of pre-cancerous cells is dealt with. If abnormalities are detected in a smear test, you may be referred for a colposcopy. This is a test that uses a microscope to closely inspect the cervix. CIN is one such abnormality that a colposcopy can detect. Mr Angus McIndoe, a leading gynaecologist, explains what CIN is and how they can be treated.
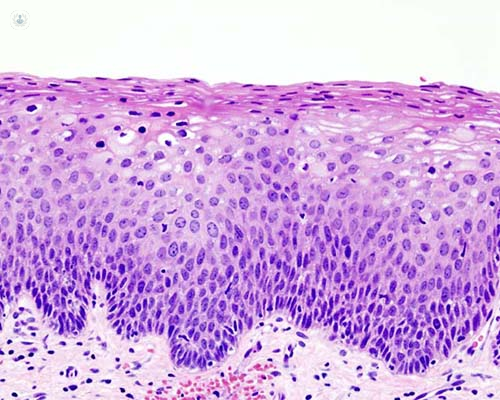
What is CIN?
CIN stands for cervical intraepithelial neoplasia. It sounds like big long medical words, but it is easy enough to understand if you take it apart. Cervical means it is on the cervix, intra means it is within, epithelial is skin, and neoplasia is cells growing faster than they should be. Therefore, cervical intraepithelial neoplasia just means that there are some cells in the skin of the cervix which are growing a bit faster than they should be.
How is CIN treated?
CIN is graded as low grade or high grade, or CIN 1, 2 and 3. With a low-grade abnormality, which is CIN one, we tend to watch and wait (i.e. we do not treat them at all). With a high-grade abnormality, CIN 2 and 3, what we do is remove them by cutting out the little bit of skin that is abnormal. This can be done in a variety of ways:
- With loop diathermy, commonly called LLETZ or LEEP.
- With a needlepoint, which allows you to very precisely cut out just the bit of skin that is abnormal.
- We can also use laser to remove the abnormality, or many years ago, people used to use a scalpel to cut it out, but very few people do that nowadays.
- The alternative treatment is an ablation where people use heat treatment to kill the cells that have the CIN.
Hence, we are able to tailor the treatment much more to the individual woman and individual abnormality that they have got. One problem with the ablation method is that you may not know what exactly has been treated, and occasionally, this kind of treatment misses an early cervical cancer. Therefore, most of us feel that excisional techniques are the better option.


