Colon polyps and the polypectomy procedure
Written by:After learning that you or a close friend or relative has received a diagnosis of colon polyps, you might start to worry. However, these are actually very common and can be removed during a routine procedure, which is called a polypectomy. Dr John Martin, a gastroenterologist, explains all you need to know about polyps, treatment, recovery and the likelihood that polyps will return after removal.
What is a polypectomy?
A polypectomy is the name of the procedure used to remove polyps. This procedure is usually conducted at the time of a colonoscopy.
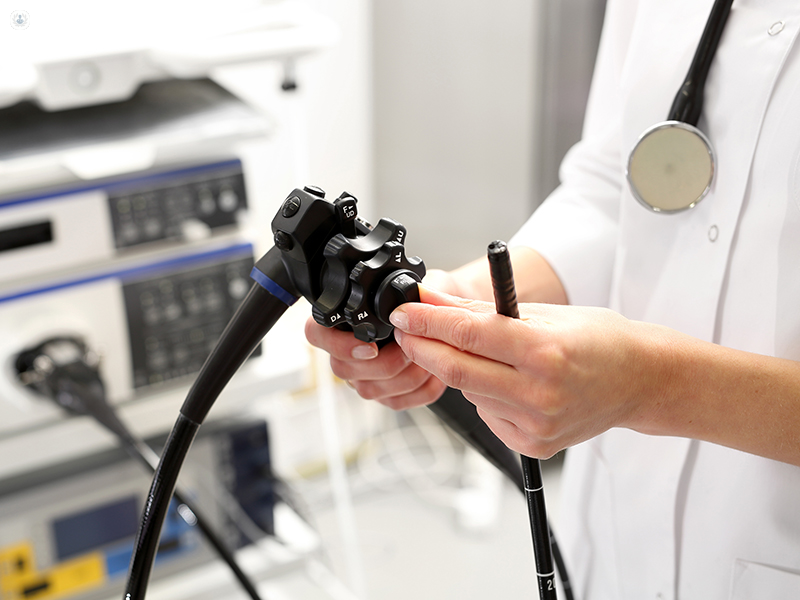
During a colonoscopy and polypectomy, an endoscope (a camera for inserting into a natural opening of the body) is inserted into the rectum and along the colon in order to check for abnormalities. One of these abnormalities can be one or several polyps.
During the procedure, the patient will be under conscious sedation. This means that while the patient is awake during the procedure, a combination of sedatives and anaesthesia ensures that they will not feel pain, at most it may be uncomfortable.
Who needs a polypectomy?
Anyone who has been diagnosed with a polyp will require a polypectomy to remove it. Polyps are commonly found during colonoscopy or a virtual colonoscopy, a special type of CT scan that examines the colon.
Who is most likely to have polyps in their bowel/colon?
Anyone can develop a polyp, but below are some of the factors that increase the likelihood of developing one:
- Age
- Genetics
- Certain foods (such as red meat and processed meat)
- Smoking
- Alcohol
While anyone can develop polyps, the likelihood increases with age. It is worth considering a screening colonoscopy at the age of 50 years, even in the absence of symptoms. Younger people, however, should be aware that they can develop polyps too and should see a doctor if they have symptoms such as changes to their bowel habit or rectal bleeding, or if they have family members with colon cancer or polyps.
Fruit and vegetables can help lower the chance of developing polyps, but genetics play a strong role and you can still have polyps despite having a healthy diet.
Are polyps a sign of colon/bowel cancer?
Some polyps predispose to bowel cancer, meaning that while they are simply a growth, there is the possibility that they will eventually turn into cancer. In fact, about 10% do. Small polyps are less likely to turn into cancer and will take longer, whereas larger ones are more likely to become cancerous and will do so faster.
Polyps are nearly always removed to prevent cancer, but if a doctor is completely confident that the polyp is not the type to develop into cancer, he or she may leave it. However, in any case of doubt, it will be removed.
Will I need to do anything before the procedure to prepare?
The preparation is the same as for a colonoscopy; you will need to drink only liquids during the 24 hours before the procedure and take a solution that will help you empty your bowels. Furthermore, you will need to stop taking any blood thinning medication; a specialist will confirm if you should stop taking any blood thinners, however aspirin is still fine.
Are there different possible ways to carry out the procedure?
Polypectomy is a term used for a range of procedures and the removal method depends on the size of the polyp. Very small polyps will be taken off routinely by anyone, and specialists with more expertise will remove larger polyps. Furthermore, some polyps are so small that they can be pulled off, while others require different techniques.
Most polyps are removed with a polypectomy snare, a tool that opens to make a loop that is placed around a polyp and then closed, ultimately cutting off the polyp. Heat can also be used with the polypectomy snare to help cutting and also to reduce the chance of any bleeding.
After the procedure, polyps are always sent for analysis. A pathologist will examine them and the doctor will provide you with the results
What are the risks of a polypectomy?
A polypectomy is fundamentally a small surgery in the colon so there is a small risk of bleeding or damage to the colon. The risk of these increases with the size of the polyp and removal of small polyps is almost risk-free.
There is a higher, but still small, risk of complications when removing a large polyp, but the likelihood of these turning into cancer is very high and the risk of removal is much lower than the risk of leaving the polyp behind. The alternative to polypectomy for large polyps is surgery and your doctor will discuss the advantages and disadvantages of both approaches with you.
Does it take a long time to recover after a polypectomy?
Patients recover immediately and are usually in and out of the hospital/clinic within a few hours.
What are the chances that the polyps will return?
The likelihood that polyps will return depends on the size and number of polyps found.
- Three to six months after a polypectomy, you may be asked to visit your doctor to check that the polyps are fully removed. This is only necessary if a large polyp has been removed.
- You’ll be strongly advised to have another check-up to ensure that you do not develop further polyps. This may be in either one, three or five years, and your doctor will advise you when this is necessary.
Dr John Martin is a highly experienced gastroenterologist and an expert in all aspects of gastroenterology. If you would like to know more about this procedure or any topic related to gastroenterology, visit his profile to make an appointment.


