How much do you know about Keratoconus?
Written by:When people mention eye conditions, we think of things like short-sightedness, cataracts and glaucoma. One that often gets missed off the list is keratoconus. As November 10th is World Keratoconus Day, Top Doctors and expert ophthalmic surgeon Vincenzo Maurino bring you the facts you need to know about KC.
What is keratoconus?
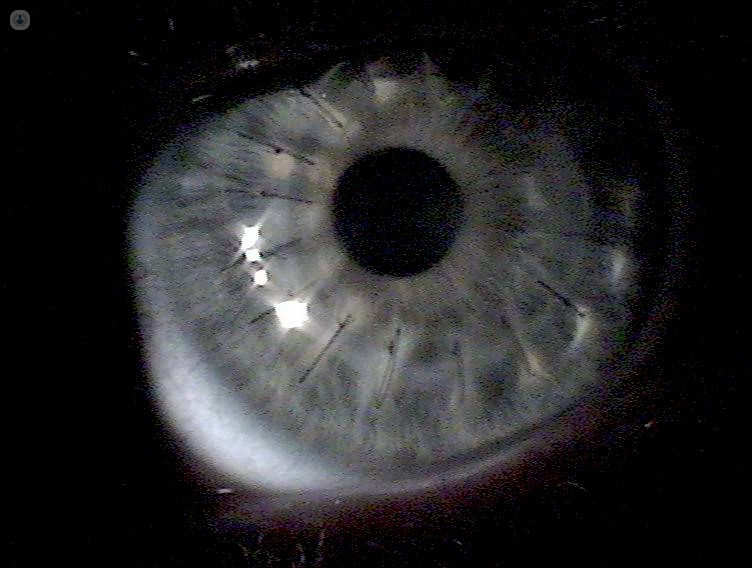
Keratoconus is a progressive eye disorder affecting the front part of the eye: the cornea.
The cornea is the window of the eye that allows the light to come inside the eye in a particular angulation and thus needs to be transparent and with a regular shape.
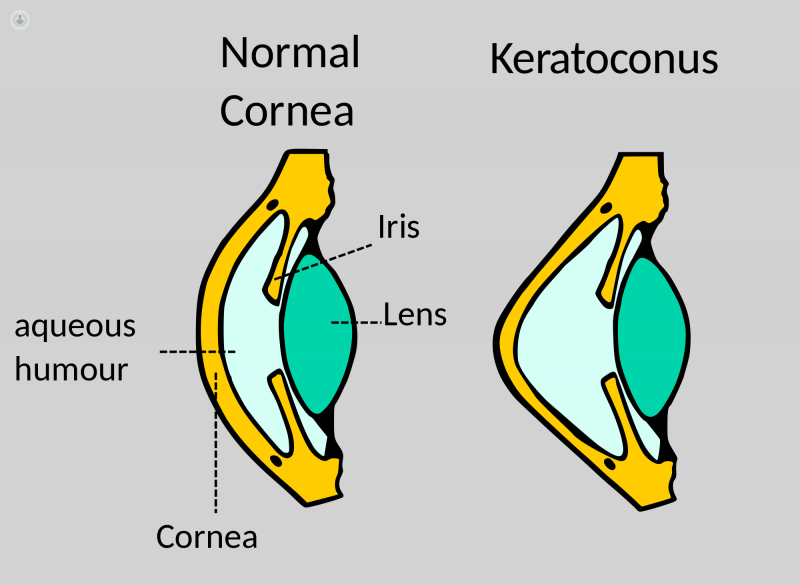
In keratoconus, the cornea becomes thinner and its shape begins to distort, bulging into a cone-like shape instead of its natural round appearance. When affected by keratoconus, the new shape of the cornea changes the way it bends light onto the retina, and as a result sight becomes blurred. Keratoconus usually occurs both eyes and often one eye is more affected that other.
Did you know…?
- The cornea is responsible for about two thirds of the eye’s optical power; the lens, which focusses light, is responsible for the remaining third.
- Keratoconus occurs in all ethnic groups and in all parts of the world.
- Roughly 1 in every 2,000 people are affected by keratoconus.
- Keratoconus often develops in a person’s teens or early twenties and tend to stabilize during the third decade of life
- If keratoconus is not treated, vision can deteriorate significantly
What to watch out for: the top 5 signs of keratoconus
- Blurred/distorted vision
- Near-sightedness
- Astigmatism
- Light sensitivity
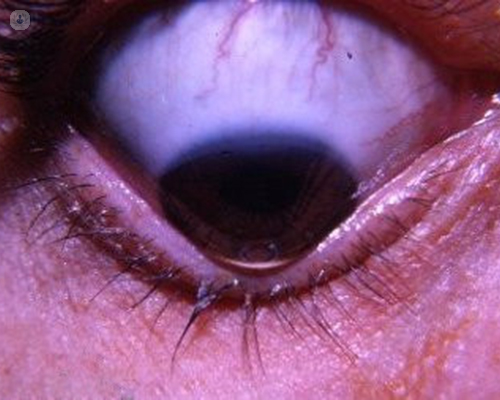
- Scarring or a circular shape visible in the cornea (severe cases)
If you are experiencing symptoms of keratoconus, you should visit your doctor or a specialist.
Can keratoconus be corrected?
Mild forms of keratoconus can be corrected by prescription glasses or soft contact lenses to combat the short-sightedness. In most patients, the disease stabilises within a few years without progression to serious sight problems, but more serious cases, such as when the cornea becomes scarred, require more serious responses. Special types of lenses, such as scleral lenses and “piggyback” lens combinations may be recommended to improve vision.
Corneal Graft and cross-linking
In serious cases, correction may no longer be possible, and a corneal graft may be necessary (20% of affected eyes).
A more recent development for the treatment of keratoconus is corneal collagen cross-linking – a treatment that aims to strengthen the cornea to prevent progression of the bulging caused by keratoconus. It is important to highlight that as cross-linking aims to stop the progression of keratoconus it is better to perform it when the disease is still at its early stage. Young patients with early diagnosis of keratoconus and signs of clinical progression are the ideal candidates for corneal crosslinking.
Novel surgical techniques also use cross-linking combined with the excimer laser to attempt to correct the abnormal corneal shape of keratoconus and at same time to strengthen, in order to achieve better vision with glasses. However, these new techniques are indicated in only a few patients, and patients need to be carefully examined and counselled before considering these options.
Keratoconus monitoring is based on three-dimensional serial measurements of the cornea with a corneal tomography instrument called a “pentacam”, which is the gold standard in diagnosing and monitoring KC patients.
November 10th is World Keratoconus Day – the perfect time to spread awareness of KC.


