How to treat thyroid eye disease (TED)
Written by:Thyroid eye disease (TED) is an uncommon and complex eye condition that can often be very distressing for anyone suffering from it and occasionally sight-threatening. It is characterised by progressive inflammation, swelling and damage to the tissues surrounding the eyes, and treatment depends on the severity and phase of the disease.
We asked Mr Jimmy Uddin, the leading consultant ophthalmologist who runs the “TED” clinic at Moorfields Eye Hospital, London and has over 20 years extensive experience in treating thyroid eye disease, to explain more about it, what the main symptoms are and how it can be treated.

What is thyroid eye disease?
Thyroid eye disease, also known as Graves' eye disease, is an orbital condition that affects the eye and face in which the fat and muscles around the eye become inflamed, swollen and sometimes “stiff”. It is often autoimmune and associated with systemic/overactive thyroid problems in up to 90% of patients. While some patients do not have systemic thyroid problems, many can go on to develop them within a year.
Classically, it is important to recognise the phase and severity of TED, but it is also important to categorise the different types (phenotypes) of thyroid disease so the correct and most effective management plan can be offered.
Who develops the condition?
It largely affects people with a systemic or overactive thyroid (hyperthyroid or Graves’ disease). It is also more common in young to middle-aged women - up to 3 or 4 times more common. It can be severe in the older patient group and is more likely to develop in people who smoke, who will also have a more severe and treatment-resistant disease.
What are the symptoms of thyroid eye disease?
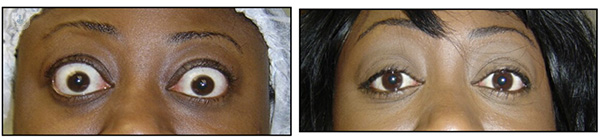
Most patients have mild or moderate disease with a starey appearance, puffy upper and lower lids, and protruding eyes (proptosis). The eyes can ache and be red, sore, watery and may not close properly. Double vision indicates more moderate to severe disease.
For patients who have more severe disease, their symptoms usually progress quickly in a matter of weeks or a few months. For those with mild to moderate disease, it tends to be more insidious and progresses slowly over months. Patients with a very quickly progressing form thyroid eye disease tend to have worse symptoms. These include:
- The feeling of irritation or grittiness in the eyes
- Redness and inflammation
- Puffy upper and lower lids (as well as the brow and face)
- Pain behind the eye upon movement
- Excessively teary eyes (sometimes worse in the morning)
- Bulging of the eyes
- Double vision
- Sensitivity to light
- Occasionally, it can lead to a reduction in vision
Psychological impact
TED can be very distressing for the patient as the condition not only affects the eyes but can change the whole appearance of their face, including the skin and eye-brows. For example, due to the inflammation, it can cause the patient’s eyes to appear starry and bulgy, leading others to misinterpret them as being angry. In addition, other people may begin noticing the changes to their facial appearance before the patient even does. All of this can have a significant psychological effect on the patient, making it difficult for them socially and professionally and to come to terms with their changing appearance.
How can TED be treated?
To treat thyroid eye disease, an appropriate diagnosis is needed. This may include examining the eyes through ophthalmology tests to investigate the severity of the condition and inflammation, and carrying out blood tests for thyroid antibodies and investigations using a CT or MRI scan. Depending on the progression and the phase, the appropriate treated can then be used.
There are two to three phases of thyroid eye disease:
- Early, active or “wet” phase — can last three to 12 months
- Mid plateau phase — the disease is not changing much and can last many months
- Late phase, burnout or “dry” phase — after 12 to 18 months
If thyroid eye disease is caught in the early phase, you can undergo disease-modifying treatments in addition to controlling the risk factors e.g. stop smoking and control the systemic thyroid activity and any other associated factors such as diabetes and blood pressure.
If the disease is caught during the active inflammatory phase, you may treat any dryness and swelling by using artificial tears and anti-inflammatories. The surface of the eye may be dry due to the inflammation in tear glands and exposure.
With moderate to severe cases, some patients will also need to receive intravenous steroids on a weekly basis for about 12 weeks. This is a proven and approved method of treatment and disease-modifying, benefiting over 70% of patients in this group.
If you have severe disease, you will need to undergo more aggressive treatments such as drops, ointments and the use of a moisture chamber (a strategy using cling film or eyeglasses to slow the evaporation of tears from the ocular surface). Other treatments can include radiotherapy and occasionally surgery.
There are other treatment options, which include the use of Rituximab and other immunological agents. Furthermore, Tepezza (Teprotumumab) is a promising new treatment option but is not available in the UK at present. A study into the drug concluded that “among patients with active thyroid eye disease, teprotumumab resulted in better outcomes with respect to proptosis, Clinical Activity Score, diplopia, and quality of life than placebo; serious adverse events were uncommon”.
When would you need surgery for TED?
Surgery is commonly performed in the late or burnt-out stage of the condition. It forms part of the staged aesthetic and functional rehabilitative surgery plan to restore the look and function of the eyes.
Sometimes, surgery may be needed in the early stage of thyroid eye disease to treat severe exposure problems (corneal problems and dry eyes). Likewise, if the disease is severe or your vision is affected, then we would need to look at carrying out decompression surgery to reduce pressure on the optic nerve and improve the appearance of the eyes.
What are the surgical options?
Surgery is used for aesthetic and functional rehabilitative purposes. We do it when the disease has burnt out and stopped progressing (usually one to two years after the start of the disease). There are four types of surgeries which can be used:
1. Decompression surgery — removal of some of the bone and fat around the eye to allow the eye to fall back to a more natural position. This helps to improve the bulging appearance of the eyes and reduces the puffiness of the lids and lacrimal gland. This needs to be tailed to the disease type (muscle expansion/fat expansion), eye movement problems, degree of proptosis, etc.
2. Squint surgery — performed to improve double vision and correct a squint. It involves moving the muscles attached to the eye to a new position.
3 and 4. Lid surgery (upper eyelid lowering, lower eyelid raising and blepharoplasty) — this is carried out to reposition the eyelids. If your eyes are particularly starey, lid surgery on both the upper and lower lids can help improve this. This can be done through an anterior or posterior approach. Modified blepharoplasty can help reduce swelling above the lids and brow, as well as reshape the eyelids.
Sometimes, decompression surgery and lid surgery can be combined. Lid reposition surgery is often very successful but occasionally, some people need a second or third operation (in 10% of cases) to correct minor problems, as the results are not always predictable the first time around.
What is the success rate of surgery?
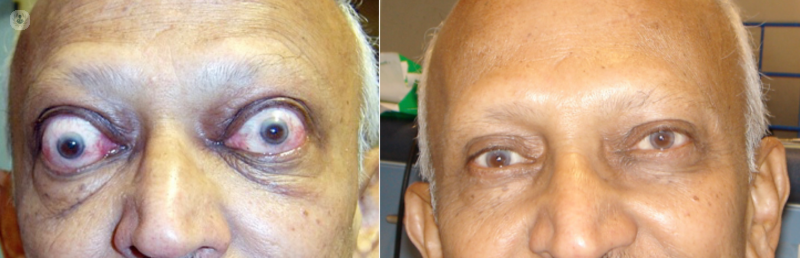
At Moorfield’s Eye Hospital, we have shown that there is a significant improvement in patients’ overall quality of life following surgery for TED. Decompression surgery is very successful in reducing the bulging and prominence of the eyes, thus improving both the physical and psychological effects this disease has on patients.
In terms of complications, there have been some reported complications of partial vision loss however, I personally have never had anyone with loss of vision during or following surgery. I am one of the most experienced decompression surgeons in the UK, having performed and presented results of over 500 surgeries (over 10 years). I also run the TED clinic at Moorfield's Eye Hospital where we have seen over 5,000 patients over 15 years.
I am confident and experienced in treating complex thyroid eye disease and performing appropriate and timely surgery, so patients can always expect the highest degree of care, attention and expertise in this area.
If you are suffering from thyroid eye disease and looking for a highly-experienced surgeon to help manage and treat your condition, visit Mr Jimmy Uddin’s Top Doctors profile and book a consultation with him.


