Achilles tendon
Mr Matthew Solan - Orthopaedic surgery
Created on: 06-27-2013
Updated on: 08-17-2023
Edited by: Karolyn Judge
What is the Achilles tendon?
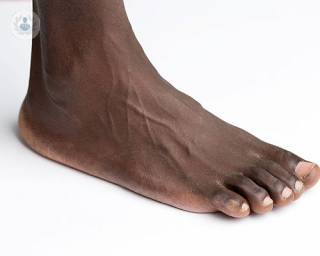
The Achilles tendon, also known as the calcaneal tendon, is the tendon that connects the calf muscle on the back of the leg to the heel bone. It is a tough band of fibrous tissue that allows the calf muscle to move the foot and is essential for walking, running and jumping.
It is the strongest and largest tendon in the body, allowing it to withstand the tension caused by movement and to bear the weight of the rest of the body. In spite of this strength, the constant high tensions it endures and its limited blood supply mean that it can suffer from several injuries and conditions.
What conditions affect the Achilles tendon?
- Achilles tendinopathy – tendinopathy is a general term for diseases of a tendon. Achilles tendinopathy encompasses Achilles tendonitis and tendinosis.
- Achilles tendonitis – an inflammatory condition caused by gradual wear and tear of the Achilles tendon due to repetitive strain or sometimes by a sudden injury. It usually manifests as pain and/or stiffness at the back of the heel where the tendon connects to it. It can take weeks or even months to heal. The RICE technique (rest, ice, compression, elevation) may help to speed up recovery, but sometimes further treatment, such as physical therapy or even surgery in certain long-term cases may be required.
- Achilles tendinosis – a gradual thickening and stiffening of the Achilles tendon with no apparent inflammation. Although it becomes thicker, the tendon is actually left more vulnerable to injury due to micro-tears caused by repetitive action. Symptoms include long-term pain, similar to tendonitis. Tendinosis is degenerative.
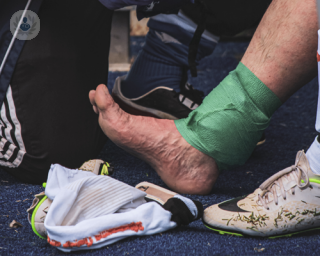
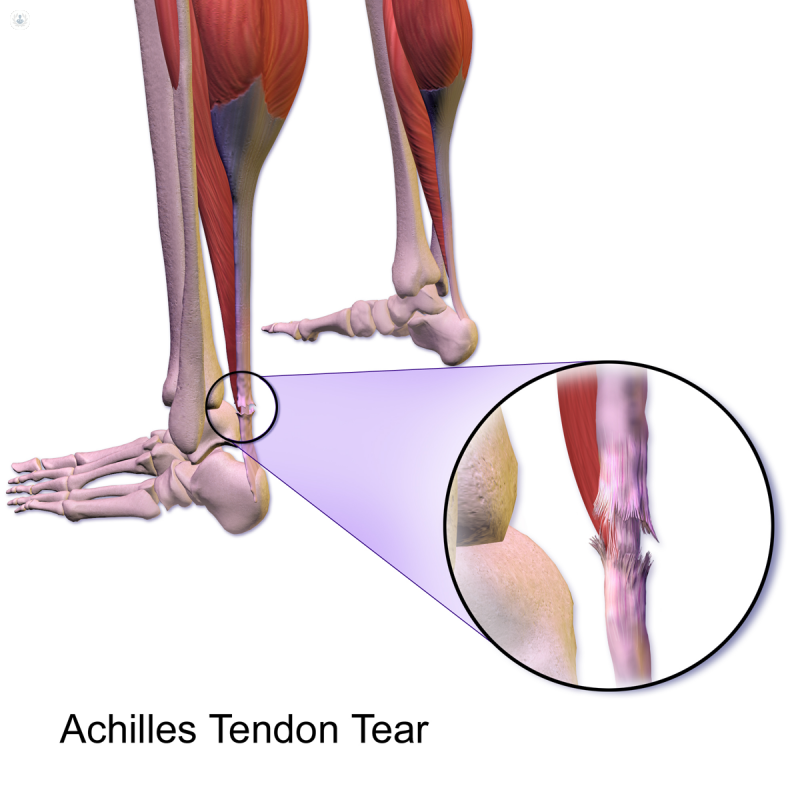
- Achilles tendon rupture – a severe injury, the tendon actually snaps, causing excruciating pain and permanent disability if left untreated. Ruptures are uncommon, occurring more often in middle-aged and older people, as in younger people, the muscles tend to tear before the tendons do. Achilles tendon ruptures may result from direct trauma, landing awkwardly after a fall or jump, or strenuous physical activity if you are not physically conditioned for it. You may hear or feel a pop and will likely be unable to bear weight with the affected foot. You should head for the emergency room immediately if this occurs. Treatment may involve the RICE procedure, immobilising the foot for 4-8 weeks, or reattaching the tendon surgically.
- Achilles peritendonitis – similar to tendonitis, but the inflammation affects the tissue around the tendon a few inches above the heel, rather than the tendon itself.
- Achilles bursitis – the bursa is a sac of fluid that cushions the tendon where it meets the heel. This can be irritated, for example by low-riding shoes, which can cause pain.
Medical tests to diagnose problems with the Achilles tendon
There are several ways to test for Achilles tendon issues:
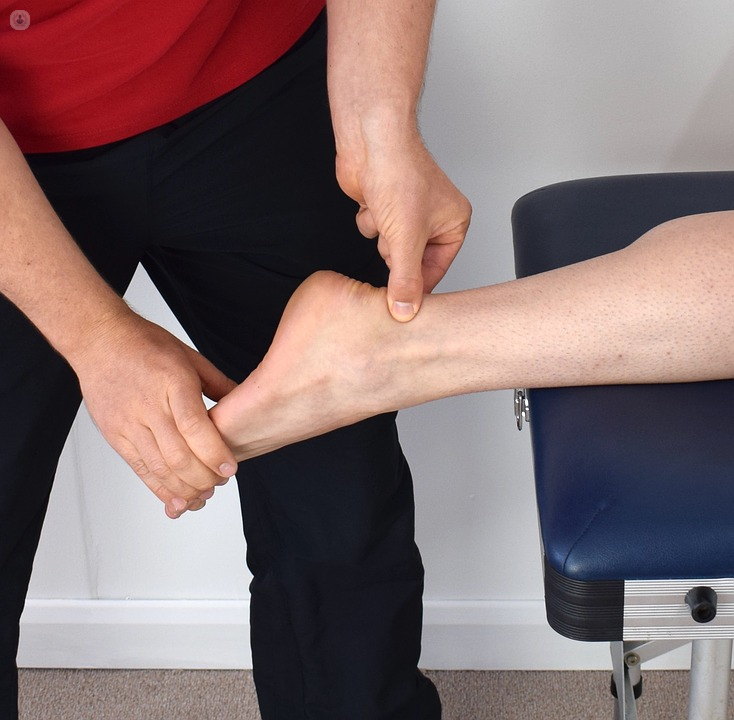
- Physical examination – most cases are diagnosed by the doctor physically examining the patient’s leg and heel, checking for pain, swelling, warmth, discolouration, thickening, or the presence of knots or lumps along the tendon.
- Thompson test – the patient lies on their stomach while the doctor squeezes their calf. The foot should move down in response if the tendon is attached. If not, it may indicate a rupture.
- MRI – magnetic resonance imaging scans can show detailed images of the condition of the tendon, and is useful for diagnosing ruptures. It may not be able to show tendinitis or tendinosis, however.
- Ultrasound – these scans use sound waves to create images and can often identify ruptures.
- CT scan – multiple X-rays are taken to scan the patient. However, MRIs are superior in identifying Achilles tendon problems, so CTs are used less frequently for this end.
Which type of specialist treats the Achilles tendon?
Orthopaedic surgeons, particularly those specialising in foot and ankle problems deal with all sorts of conditions affecting the Achilles tendon.