Corneal graft: which eye conditions affect the cornea?
Written by:The cornea is the clear window in the front of the eye and is considered the strongest lens in the eye as it contributes to about two-thirds of the eye’s total power. Any alteration with the cornea’s clarity or regularity would have a significant effect over vision.
Here, one of our top ophthalmologists Mr Radwan Almousa explains which conditions may affect the clarity of the cornea and whether donor corneas can replace those which become diseased.

How is corneal structured?
The corneal is made of five main layers: epithelium with the basement membrane, Bowman’s layer, stroma, Descemet’s membrane and the endothelium.
The tear film is the liquid layer adherent to the front of the cornea. Any alteration with this smooth liquid layer could affect the clarity of the vision, like in the case of dry eyes.
Which conditions could affect the clarity of the cornea?
The cornea is prone to bacterial infection, viruses and protozoa. The most common cause of corneal infection is a contact lens, which usually causes bacterial infection.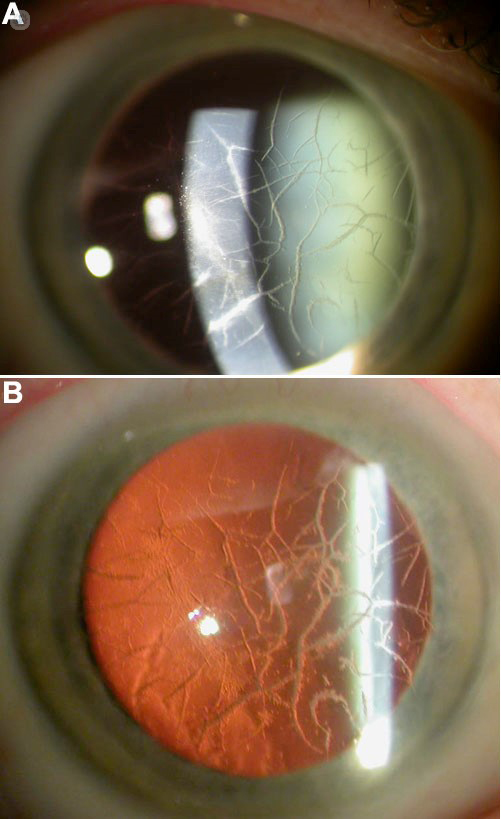
The infection rate with contact lens could be as high as one in 100 over 30 years of use and it could cause significant vision loss in one in 2,000.
Corneal dystrophies are a group of hereditary corneal diseases that could affect single or multiple layers of the cornea and might interfere with the vision.
The most famous of corneal dystrophies are the ones that affect the anterior corneal stroma and Bowman’s layer, such as Lattice dystrophy and granular dystrophy. Also, Fuchs’ dystrophy affects the endothelium layer. Both image A and B to the right shows lattice dystrophy.
Keratoconus is also a condition that could affect the clarity of the corneal. The usual corneal shape is almost spherical. In cases of ectatic corneal disorder, however, the cornea becomes thinner with protrusion and distortion of the anterior corneal surface. This leads to disturbance of vision. Keratoconus is more common in the Middle East and is associated with ocular surface allergic conjunctivitis.
Can donor corneas be used to replace diseased corneas?
When the cornea loses its clarity or if the shape of the cornea becomes irregular to the point that conservative measures, such as spectacles or contacts, are not adequate to improve the sight, the cornea could be replaced.
What’s the success rate of corneal transplantation surgery?
There is a different variety of corneal transplant procedures. The one that is chosen for the patient depends on the individual circumstance of the corneal disease that they have and the layer of the cornea that needs to be replaced. The visual outcome varies depending on the surgical procedure. The survival rate of corneal graft varies significantly depending on the types of graft and the corneal disease.
Are there different types of corneal graft and when are they used?
There are several different types of corneal graft, each used depending on the layer(s) of the cornea involved in the disease. These include:
- Penetrating keratoplasty (PK) (full-thickness graft) is used when there is severe corneal scarring, for example in cases of bacterial keratitis. The resulting scar is full thickness and therefore requires a full-thickness graft.
- Anterior lamellar keratoplasty is used when there is a corneal disease that does not affect the endothelium layer. An example of this type of graft is the Deep Anterior Lamellar Keratoplasty (DALK) where the endothelial layer is preserved.
- Femtosecond laser-assisted anterior lamellar keratoplasty (FSALK) is used when the corneal disease is confined to the anterior third of the cornea.
- Endothelial keratoplasty is used when the endothelial cells are affected by a genetic disease, such as Fuch's disease or damage that has resulted from intraocular surgery, such as in cataracts surgery. Both result in clouding and scarring of the cornea.
- Descemet’s stripping endothelial keratoplasty (DSEK) is used when the swollen cornea reaches the point of affecting the patient’s vision. This type of graft is needed to replace the endothelial layer.
- Descemet’s membrane endothelial keratoplasty (DMEK) is used when the endothelial layer must be replaced along with the Descemet's in order to clear the cornea. It can be used instead of DSEK.
Are there any risks in having a corneal graft?
Corneal graft has few complications, however as a rule of thumb, a partial thickness graft has reduced rate of complications and has less interference with the strength of the cornea.
Book an appointment with Mr Almousa now if you would like to discuss your corneal transplantation options.


