What to do with swollen veins: varicose vein treatment
Written by:Varicose veins can be a real pain – these swollen and twisted blood vessels don’t work properly and can lead to a variety of problems. Leading vascular surgeon Ms Sophie Renton explains the options for treating varicose veins.

Conservative management – compression stockings
Varicose veins form due to an increase in pressure in the veins. This in turn causes the vein to bulge and contort. Many of the associated symptoms are caused by this imbalance of the pressure inside the vein – blood cannot be efficiently pumped back up from the legs to the body.
Compression stockings counteract this by applying pressure to the outside of the leg. They tend to be tighter at the ankle than at the calf, which helps the veins to work better in carrying blood back up to the body, relieving discomfort in the leg. To control the symptoms, they should be worn all day.
Below-the-knee socks tend to be more popular than full-length stockings, and are also sold as “flight socks”, as they help to prevent deep vein thrombosis (DVT) while flying.
Endovenous laser therapy & radiofrequency ablation
Usually performed under local anaesthetic, these minimally invasive procedures are designed to avoid the need for open surgery. A thin wire is fed through the vein, guided by ultrasound imaging. Heat is applied to the site, destroying the lining of the varicose vein, which closes in on itself.
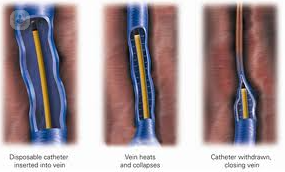
and the vein shuts down.

There are also new alternatives, like mechanochemical ablation (Clarivein™), which are relatively painless and so don’t require anaesthetic.
Another novel technology is the Sapheon closure device. This seals the vein using glue.
Foam sclerotherapy
A foam solution is injected into the vein, causing the walls of the vein to stick together. The collapsed vein eventually becomes scar tissue. The procedure takes around half an hour, and more than one session may be needed. It is usually performed on an outpatient basis.
Foam sclerotherapy is relatively painless and is an effective option for recurrent varicose veins and isolated varicosities. However, it is not suitable for all varicose veins.
Surgical treatment
Surgery may be an option if other treatments are unsuccessful or aren’t possible.
First, the junctions where the main varicose vein meets the deep vein are tied off at the groin and the knee via small incisions. This disconnects the varicose vein. Then, the trunk of the varicose vein is stripped out. Local varicosities can be removed via small incisions.
According to NICE guidelines, endovenous treatments should be considered first due to the fact that there is a high incidence of minor complications associated with varicose vein surgery. These include bruising, infection, damage to small nerves (which are responsible for feeling in the skin), and damage to the lymphatic vessels.
I rarely offer open surgery as I believe the alternatives are better.
Learn about varicose vein treatment in action in Ms Renton's case study
If you would like some expert advice on your best options to deal with varicose veins, book an appointment with Ms Sophie Renton at her profile.


