What is causing my dry eyes?
Written by:Dry eyes are usually caused by a lack of quality tears, leaving your eyes stinging and feeling uncomfortable. There are many reasons why this could happen to you and there are also many treatments available to relieve it. So we spoke to Mr Anant Sharma, a prominent ophthalmologist based in Bedford, to understand more about the main causes and symptoms of this eye condition and what options you have to treat it.

What are the main causes of dry eyes?
There are generally two main causes of dry eyes: your eyes aren’t producing enough tears to lubricate and nourish the eye surface or you are experiencing a condition known as evaporative dry eye (EDE) which causes tear instability with poor spreading and increased tear evaporation. Although it is often a combination of both, one condition usually predominates.
Common conditions causing insufficient tears are usually from medical drugs or autoimmune conditions such as Sjogren's syndrome. When EDE is present, the commonest cause is meibomian gland disease (MGD)/blepharitis which can be associated with facial rosacea.
Ultimately, dry eyes are a result of interference with the lacrimal functional unit (LFU). This consists of the lids, the surface of the eyes, tear glands and the connective nerves. If any part of the LFU is affected, it can influence the whole tear system and lead to dry eye and sometimes altered sensation.
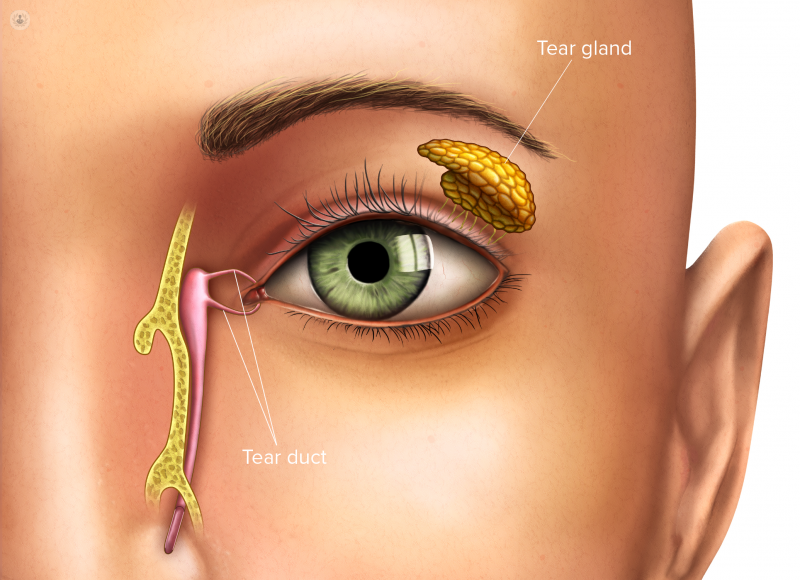
There are many underlying causes of dry eyes, however, your lifestyle and environment strongly influence the condition. These are some environmental causes:
- Dry, hot or windy climates can exacerbate tear evaporation
- Too much exposure to smoke or pollution
- Failure to blink enough from staring at a computer screen for too long
- Long term use of contact lenses often contribute to drying of the eyes
- Lack of sleep can cause many problems with your eyes and dry eyes can be one of them
- Poor diet, lack of exercise and poor hydration can also cause dry eyes
As well as environmental factors, there are also possible underlying medical/surgical causes. For example:
- Laser corrective eye surgery
- Diabetes can cause dry eyes
- Certain eye drops, especially those that contain preservatives, can cause dry eye
- Dry eye can be a symptom of some autoimmune diseases such as Sjogren's syndrome, rheumatoid arthritis and systemic lupus erythematosus (SLE).
Dry eye is more common as we age and in women more than men, as hormonal changes can cause dry eyes. Although a common assumption exists in the literature that menopause is associated with increased occurrence of dry eye, definitive evidence is lacking.
Can dry eye symptoms come and go?
Yes. As we mentioned, your environment can strongly influence the condition. Classically, dry eyes worsen towards the evening as the eyes have been open for longer and sometimes at night, due to reduced tear production and/or exposure. The time of day your eyes start feeling dry can give you a clue as to what in your surroundings may be causing it. For example, you may notice that your eyes feel drier around your contact lens wear or after being somewhere where there’s air-conditioning.
What other symptoms can accompany dry eyes?
Apart from your eyes being uncomfortable, you may also experience:
- A burning or stinging sensation
- Itchy eyes
- Red, bloodshot eyes
- Sensitivity to light
- Stringy mucus
- A gritty, scratchy feeling or the sensation of a foreign body in your eye
- Blurry vision
Can dry eyes indicate a serious condition?
Yes but this is uncommon. Serious conditions include Sjogren's syndrome, which can present with other symptoms such as a dry mouth.
What happens if dry eyes are left untreated?
The vast majority of people suffer unnecessarily because they aren’t getting the appropriate treatment. Very rarely it can affect your vision if not adequately treated, due to corneal ulceration. Often asymptomatic or mild dry eye can flare up with symptoms following an episode such as long days working at a computer screen, air conditioning or eye surgery. Pre-treatment of mild dry eyes before cataract surgery, particularly with a multifocal implant, may be required for an optimal visual outcome.
What treatments are available for dry eyes?
The initial treatment should be identifying and looking at adjusting the particular lifestyle and environment factors we mentioned above. Nutrition, regular exercise and hydration are also important. For some people, simply massaging the eyelids and/or maintaining good lid hygiene can help. If this fails, there are many treatments available. Persisting with some treatments particularly anti-inflammatories eye drops often improves symptoms.
- Adding artificial tears — You can use mild over-the-counter preservative-free eye drops. Mostly these drops have varying viscosity, adhesiveness, hydration, duration and oils. After a discussion with your doctor, they may recommend a specific artificial tear depending on the origin of your dry eye. These drops can provide an instant but sometimes temporary benefit. Be careful not to overuse them (such as hourly drops) as this can result in what’s known as the washout syndrome: This is where you can wash out all the healthy natural tears in your eyes and this can cause your eyes to feel even drier. Natural, healthy tears are always the best and restoring your eye to this balance is important, which can sometimes be done in with lifestyle/environmental changes.
- Prescription eye drops — there are many types of eye drops available and not only do they add lubrication to your eyes but can also reduce any inflammation such as ciclosporin and azithromycin. Oral drugs such as doxycycline may also be used to reduce inflammation. If inflammation persists then a short course of steroid drops may help.
- Treating infections — you can treat any infections with drops or lid cleaning solutions and sometimes tablets. Demodex infection of the lid margins can cause inflammation and dry eyes.
- Punctal plugs — these are small biocompatible implants (temporary or permanent) that are inserted into your punctae which are small holes located in the inner corner of your eyelids. These plugs can block these holes, preventing the tears from leaving your eye.
- Meibomian gland probing — the meibomian glands block with time and probing helps open the glands. If the meibomian gland oils are normal then I believe this offers the best way for your oils to express and spread more naturally with each blink. It also should aid oil expression by massaging the lids following a heat mask. For further information on this click here.
- Finger prick autologous blood (FAB) treatment — for patients with persistent dry eyes resistant to conventional therapy, this is a novel treatment option which you can do with an ophthalmologist's guidance. By taking a droplet of blood from a pricked finger and applying it directly to the eye, it can relieve your symptoms. If you are interested in this treatment, I have prepared a video demonstrating how it is carried out and you should contact me for more information. Natural tears are a complex fluid with hundreds of proteins compared to artificial tears, which mainly hydrate and lubricate. Tears are derived from blood and so it makes sense to use blood/serum made from blood if you are lacking tears.
There are many more treatments available such as intense pulsed light (IPL) and Lipiflow. I will discuss these new treatments in more detail in a future article.
The Dry Eye App
There is an app available for Apple devices called The Dry Eye OSDI Questionnaire which allows you to calculate your own OSDI (ocular surface disease index) score from home. The OSDI is a 12-item scale that assesses your dry eye disease symptoms and helps you to monitor your condition.
Further in-depth information on dry eyes can be found at the Dry Eye Workshop (DEWS 2 report).
To book an appointment with Mr Anant Sharma, visit his Top Doctors profile and check his availability.


