Rheumatoid arthritis
Dr Stephanie Kaye-Barrett - Rheumatology
Created on: 11-13-2012
Updated on: 11-10-2023
Edited by: Carlota Pano
What is rheumatoid arthritis?
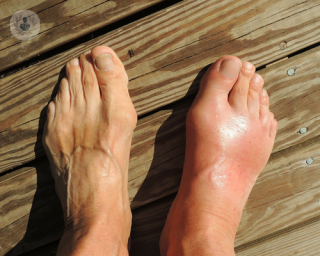
Rheumatoid arthritis is a chronic and degenerative disease that causes joint inflammation. There are certain areas of the body that this type of rheumatic condition affects more than others, which include the wrists, fingers, toes, elbows, shoulders, hips, knees, and ankles. Joint inflammation normally causes pain, deformity, and movement issues, as the cartilage wears out and the bones rub against each other.
The cause for this condition remains unknown, and there is no known cure. Damage to the bone and cartilage is irreparable, which is why treatment seeks to relieve pain and disability, as well as avoid permanent joint damage.
What are the main symptoms of rheumatoid arthritis?
Rheumatoid arthritis affects joints on both parts of the body equally. The condition starts slowly, and the initial symptoms tend to be mild joint pain, stiffness, and fatigue.
Other symptoms include morning stiffness that lasts longer than one hour. The joints may feel hot, weak, or sensitive and rigid when they are not used for a while. Joint pain is often the same on both sides of the body. In some cases, joints may become inflamed. Over time, joints may lose their range of movement and become deformed.
Some of the most common symptoms include:
- chest pain when breathing (pleurisy)
- dry eyes and mouth (Sjögren syndrome)
- burning, itching, or discharge in the eyes
- nodules under the skin
- limb numbness or tingling
- difficulty sleeping

How is rheumatoid arthritis diagnosed?
There is no definitive test to diagnose if a patient has rheumatoid arthritis, but some can help in its indication. Some of the main tests used to indicate rheumatoid arthritis include:
- full blood count
- C-reactive protein
- erythrocyte sedimentation rate (ESR)
- joint X-rays
What are the main causes of rheumatoid arthritis?
As mentioned above, the causes remain unknown. It is an autoimmune disease which involves genetic factors: a family history of the disease increases chance of developing it.
Non-genetic factors also play a big role, and these can include infections, female hormones, smoking, stress, being overweight, and the type of diet you follow.
Can it be prevented? If so, how?
There is no known way of preventing the disease.
However, some risk factors have been identified such as smoking and chronic gum infections, which can really aggravate the condition. This is why it is important to not smoke and maintain good oral hygiene.
Having a correct and personalised treatment can help prevent joint damage.
How is rheumatoid arthritis treated?
In most cases, this condition requires long-term treatment, which may include:
Different types of medication, including:
- antirheumatics
- anti-inflammatories
- antimalarials
- corticosteroids
- biological agents
Physiotherapy options include:
- joint protection techniques
- hot and cold treatments
- splints or orthopaedic devices to support and align the joints
- it is recommended to sleep between eight to 10 hours a night, and to rest between activities
Surgery is also an option. The surgical options include:
- removal of the joint lining
- in extreme cases, total arthroplasty, which may involve knee replacement or hip arthroplasty
Exercise, education, and nutrition also play an integral role in the treatment of rheumatoid arthritis.
Which specialist treats rheumatoid arthritis?
The specialists who treat rheumatoid arthritis are rheumatologists.
What are the main potential complications of rheumatoid arthritis?
Patients suffering from rheumatoid arthritis can potentially suffer severe, and in rare cases, life-threatening complications. These can include the following:
- carpal tunnel syndrome
- inflammation of the lungs
- inflammation of the heart
- inflammation of the eyes
- increased risk of heart attack and stroke
- cervical myelopathy
- joint damage
Is rheumatoid arthritis hereditary?
There is a certain genetic component in a select few of patients that increases one's risk of being diagnosed with rheumatoid arthritis.
What is the prognosis?
If the condition is not managed appropriately with adequate and prompt treatment, patients can eventually end up developing jont deformity and disability. Some patients, depending on how severe their diagnosis of rheumatoid arthritis is, may be forced to give up their job.
Having said that, many patients continue to enjoy a good quality of life even if they have been diagnosed with the condition. This is largely due to the fact that new, highly effective treatment strategies that are put in place to strictly control and manage rheumatoid arthritis have been introduced in the last couple of years.