Why are anaesthetists so important in surgery?
Written by:The anaesthetist plays a very important part in surgery and it is essential that the surgeon and anaesthetist work together to optimise surgery. The anaesthetist cares for the patient from when they’re put to sleep until they wake at the end of surgery. Mr Ahmed R. Ahmed is a leading surgeon, and here he explains that succcessful surgery not only requires a skilled surgeon, but a highly attentive and skilled anaesthetist.
During an operation, why is the relationship with the anaesthetist important?
Anaesthetists create the ideal conditions both for the surgeon and the patient, monitoring the patient's physiology throughout surgery, and responding to the surgeon’s needs or pre-empting the surgeon’s needs, thereby contributing to a successful surgery. They make sure that the patient’s physiology is maintained as near to normal parameters as is possible. This involves monitoring the heart, blood pressure levels, oxygen levels, and other factors such as implementing a pain relief strategy during the operation.
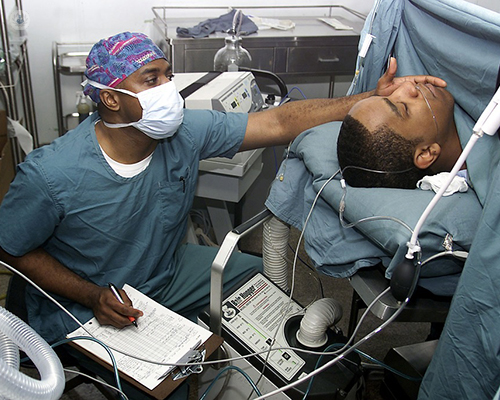
Anaesthetists do not simply ‘put someone to sleep’ but in fact play an orchestral part during the operation. They administer a number of drugs such as muscle paralysing agents. If the paralysis is not administered properly or the muscles are not in the correct state of paralysis there will not be enough room or space for the surgeon to operate, there will be excess strain and torque on the surgeon’s instruments from working against a non-relaxed abdominal wall as well as other hindering effects such as patient coughing or bucking during surgery.
The anaesthetist controls the level of muscle relaxation, called a ‘neuromuscular block’. If there is a deep muscular block then the surgeon will be able to get a better view, a more still patient and less torque on instruments while operating, therefore contributing to a positive outcome of surgery. Constant dialogue between surgeon and anaesthetist helps the operation to run as smoothly as possible.
What steps do you take together to ensure a successful surgery?
Ideally, the journey that the patient takes with their surgeon and anaesthetist actually starts from before they enter the operating theatre. The whole process should be a collaboration between surgeon, anaesthetist, and patient. This is particularly true in morbidly obese patients who are increasingly meeting their anaesthetists long before their scheduled operation is performed, rather than simply on the day or a few days before.
Anaesthetists meet the patient before the surgery to begin the collaboration. The meeting with the anaesthetist is conducted in an outpatient clinic situation so they can listen to the patient’s needs and create a broad understanding of the individual, identifying any existing health problems and optimising these before surgery.
Nowadays, we are using different techniques to help control the pain which the patient feels after surgery. For example, general anaesthesia can be used in co-ordination with a single shot spinal injection given at the start of surgery to numb the nerve fibres that carry pain even before the operation has begun. The anaesthetist can also provide a local anaesthetic solution, which they give to the surgeon, who can spray it inside the abdominal cavity to reduce pain generated internally.
In laparoscopic surgery, using a deep neuromuscular block allows the surgeon to reduce the pressure of gas they’re using to create operating working space, which in turn helps reduce post-operative pain, and in particular shoulder tip pain (a type of pain which is felt where your shoulder ends and your arm begins, and is often a type of ‘referred’ pain).
In theatre, many of us have also switched to using warm humidified carbon dioxide now instead of using the traditional cold dry carbon dioxide as the preferred agent for creating space inside the abdominal cavity. There are now machines available which use warm humidified carbon dioxide, which causes less drying to the abdominal cavity membrane and causes less post-operative complications. This is currently only available in more modern facilities, but tools, techniques, and ways of collaborative working are consistently improving surgical outcomes for patients and ensuring that we, as surgeons, are giving the best care possible.
To find out more, make an appointment with an expert.


