Knee osteoarthritis
Mr Peter Craig - Orthopaedic surgery
Created on: 11-13-2012
Updated on: 10-18-2023
Edited by: Conor Dunworth
What is osteoarthritis of the knee?
Osteoarthritis of the knee is a disease which mainly consists of a tearing of the articular cartilage, and it can be progressive.
The disease is not exclusive to old age, however, the frequency of affliction increases with age. It is also more common in women than in men, and in people who are genetically predisposed to it. Although many of these factors are not preventable, it is possible to slow down its progression or to reduce the chances of it developing.
There are two types of knee osteoarthritis: primary knee osteoarthritis, which is related to age, and secondary knee osteoarthritis, which occurs after a previous injury, such as a fracture and affects people with high levels of strenuous physical activity or those who are obese.
Prognosis of knee osteoarthritis
Although osteoarthritis is generally not a serious disease, it can gradually undermine the quality of life of those affected. Prognosis of the disease depends greatly on the pathology and its evolution. Early diagnosis and joint protection measures are key in helping to slow the progression and development of the disease. Pain and a lack of mobility are the main factors that have an impact on the person’s quality of life, causing it to decrease.
The disease mainly affects people over the age of 50. It can make them more sedentary, which can result in obesity and the appearance of risk factors for conditions such as cholesterol, hypertension and diabetes, among others.
Symptoms of knee osteoarthritis
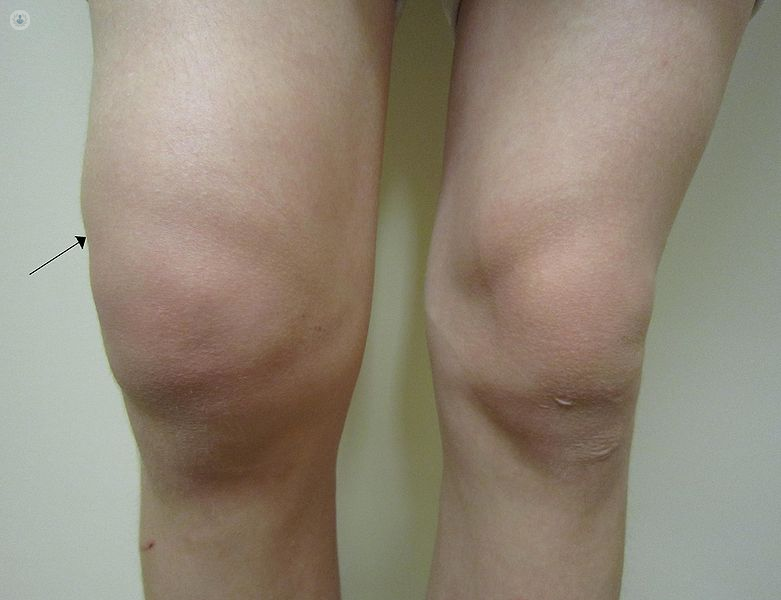
The symptoms and manifestations of osteoarthritis are diverse, progressive and appear gradually over time. The most common symptom is joint pain with limited joint movement, accompanied by cracking sounds and sometimes knee joint effusion (also known as ‘water on the knee’). Some people may experience stiffness or joint deformity.
The worst symptom is pain. In the early stage of the disease, pain occurs when you move or try to force the affected joint, and it subsides when you rest. As the disease progresses, pain can occur not only when you move the joint but also when it is being rested. However, joint pain is not constant, so you can go for long periods of time without any pain, although the disease continues to progress.
How is knee osteoarthritis diagnosed?
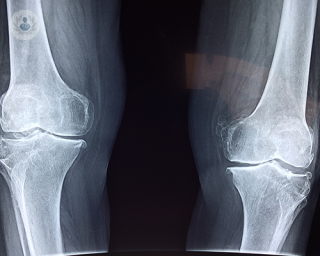
Osteoarthritis can be difficult to diagnose. Firstly, it should be noted that it cannot be diagnosed by X-ray, so a thorough medical history must be taken and a physical examination performed. If there is swelling in the knee, the specialist may decide to remove fluid from the joint to test it and to confirm the diagnosis. In addition to X-rays, a CT or MRI scan may also be used to diagnose knee osteoarthritis.
What causes knee osteoarthritis?
The cause of osteoarthritis is still unknown. However, there are a number of risk factors associated with its occurrence:
- Gender: osteoarthritis affects women between the ages of 50 and 55 in particular.
- Age: the risk of osteoarthritis increases after the age of 50
- Genetics: it may be an inherited disease
- Strenuous physical activity: constant repetition of joint movements can lead to joint overload
- Menopause: decreased oestrogen levels are a risk factor for the development of the disease
- Obesity: this can aggravate osteoarthritis in joints such as the knees
- Trauma: fractures and injuries can trigger osteoarthritis.
Can knee osteoarthritis be prevented?
The main measures for preventing the onset of osteoarthritis are simple: eat a healthy, balanced diet and take regular, moderate physical exercise according to your age and physical condition. You should limit strenuous physical exertion, such as lifting or carrying heavy objects. Contact sports such as football and rugby are not recommended for people with osteoarthritis, as they can exacerbate the disease. Footballers are one of the groups most affected by this disease due to frequent meniscus injuries.
Treatment for knee osteoarthritis
The main objective of treatment for osteoarthritis is to improve pain and functional disability. The first step is awareness, as avoiding risk factors is essential for preventing or minimising the disabling effects of the disease.
You will also have a personalised and adapted exercise regimen which you need to follow with the physiotherapist to help improve your condition.
- Anti-inflammatories: sometimes pain is severe due to inflammation of the area. In this case, anti-inflammatory drugs may be prescribed to reduce inflammation and relieve pain.
- Chondroprotective drugs: these are specifically indicated for the long-term treatment of osteoarthritis, as they act directly on the joint. They relieve pain and improve mobility, as well as attack the disease at the root by slowing its progression. Chondroprotectors include glucosamine and hyaluronic acid.
- Surgery: implant surgery will be recommended if the disease is very advanced; in this case, a partial or total knee implant.
Which specialist treats knee osteoarthritis?
There are several specialists that can treat knee osteoarthritis, including orthopaedic surgeons, rheumatologists and physiotherapists.