Pancreatic cancer
Mr Satyajit Bhattacharya - Surgery
Created on: 11-13-2012
Updated on: 09-22-2023
Edited by: Karolyn Judge
What is pancreatic cancer?
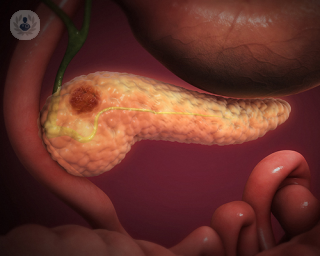
The pancreas is a large gland in the abdomen, which produces enzymes that aid in digestion. Pancreatic cancer is when abnormal cells develop in the pancreas and multiply out of control. As these cells do not function normally, they hinder bodily functions as they multiply, eventually leading to death if not treated.

Cancer can develop in different parts of the pancreas:
- Ductal adenocarcinoma develops in the lining of the pancreatic ducts (which carry the enzymes produced to the digestive system). Around 95% of pancreatic cancer cases are ductal adenocarcinomas.
- Ampullary cancer develops at the ampulla of Vater. This is where the pancreatic duct meets the bile duct before entering the intestines.
- Cystic tumours – although the pancreas can develop benign cysts (fluid-filled sacs), occasionally it grows cancerous ones.
- Neuroendocrine tumours start in the endocrine cells, which produce hormones like insulin.
- Acinar cell carcinomas develop in the cells that synthesise the pancreatic juice (the mixture of digestive enzymes).
- Lymphoma – cancer of the lymphatic tissue, which threads through the entire body, including the pancreas.
What are the symptoms of pancreatic cancer?
In the early stages, pancreatic cancer may not show any symptoms, making it hard to diagnose. Symptoms such as abdominal pain, indigestion and weight loss can manifest as the cancer develops and grows. Unfortunately, these symptoms are common and can indicate a number of other conditions. Other possible symptoms include:
- Jaundice (yellow skin and eyes, itching)
- Change in bowel habits, e.g. constipation, diarrhoea
- Nausea/vomiting
- Diabetes (especially if only recently developed or diagnosed)
What causes pancreatic cancer?
The causes are not fully understood, but certain risk factors have been identified, such as age (patients are generally 50-80 years old), smoking, and a history of certain conditions (e.g. diabetes and chronic pancreatitis). There is thought to be a genetic factor in some cases, as in about 1 in 10 cases the patient’s parent or parents also had pancreatic cancer.
How is pancreatic cancer diagnosed?
There are various tests available in order to diagnose pancreatic cancer. They include:
- Blood tests
- Blood is tested for specific proteins, or tumour markers, that are shed by pancreatic cancer cells. One type of test for pancreatic cancer is called CA19-9, which can assist is understanding how cancer responds to treatment.
- Scans
- UItrasound scans can be done from outside the abdomen (transabdominal) or via an endoscope. An endoscopic ultrasound (EUS) makes images of your pancreas from inside your abdomen via an ultrasound device. This device is passed through a thin, flexible tube called an endoscope, down your oesophagus and into your stomach.
- CT scan;
- MRI scan;
- PET scan.
- Biopsy
- A small sample of tissue is removed from the pancreas for examination under microscope, in a biopsy for pancreatic cancer. An endoscopic ultrasound (EUS) is collected by passing tools through the endoscope in order to collect the tissue. Sometimes, a sample of tissue is collected via fine-needle aspiration by inserting a needle through your skin and into your pancreas.
What is the treatment for pancreatic cancer?
Pancreatic cancer is difficult to treat, as it is rarely detected until the tumour has become quite large. Treatment depends on the type, location and size of the tumour, as well as the age and general health of the patient. If it is possible to remove the tumour completely, this is the preferred option, but in cases where this is not possible, different treatment will be recommended to contain the cancer, prevent further growth and minimise the damage it does to the body.
The three main treatments, which may be used individually or in combination are:
- Surgery
- Chemotherapy
- Radiotherapy
Recovering from surgery on the pancreas can be a long process. The patient may need support from help from dieticians and physiotherapists.
What's involved in pancreatic cancer surgery?
The most effective treatment for pancreatic cancer is surgery. It's the best for removing the cancer and can assist in you living longer, while symptoms can improve as well. However, possible complications, recovery time and side effects such as digestion problems and diabetes, are some of the disadvantages of pancreatic cancer surgery.
The pancreas has a shape like a comma, with a head and a tail. Removal of the head of the pancreas (which is usually removed along with an adjacent length of bowel called the duodenum) is called a Whipple's operation or Pancreato-duodenectomy. Removal of the tail (usually removed along with the spleen) is called Distal Pancreatectomy. Very occasionally the whole pancreas may need to be removed which is called Total Pancreatectomy. These operations may be done through an open or keyhole approach.
In open surgery for pancreatic cancer, one large incision is made in the stomach, while in keyhole surgery, several small cuts about one to two centimetres are made in the same area. An endoscope with a camera attached to it, is used to guide the surgeon. Robotic surgery is similar, but the instruments are controlled by the surgeon via a computer (not held by a surgeon's hands.) Keyhole surgery may not be suitable for everyone, and if surgeons think the operation may be more complicated, they will recommend open surgery.
What are the stages of pancreatic cancer?
The main way of staging cancers is the TNM system (Tumour, Node and Metastasis).
- Tis
This is early-stage pancreatic cancer that hasn't gone down into the deeper layers of tissue within the pancreas, and it's uncommon for pancreatic cancer to be diagnosed very early.
- T1
It means the cancer is inside the pancreas and is two centimetres or less in any direction. It is split into three stages, T1a, T1b and T1c.
- T2
This stage is where cancer is between two and four centimetres in any direction.
- T3
At the T3 stage, the cancer is bigger than four cm but is still within the pancreas.
- T4
The cancer has grown outside of the pancreas into the nearby large blood vessels at the T4 stage.
Node (N), describes whether the cancer has spread to the lymph nodes. If cancer has spread to the nearby lymph nodes, it means there is a higher risk that cancer cells may have spread further than the pancreas. N0 means there are no cancer cells in the nearby lymph nodes, N1 signifies that there are 1 to 3 lymph nodes which have cancer cells in them, N2 means there is cancer in 4 or more lymph nodes.
Metastasis (M) signifies if the cancer has spread to a different part of the body.
What are survival rates for pancreatic cancer?
That depends on the type and stage of cancer and the patient's overall condition.
Which specialist treats pancreatic cancer?
There are various specialists that may play a part in treating pancreatic cancer. These are:
- Gastroenterologists. These doctors specialise in diagnosis and treatment of digestive system conditions, and can help to control symptoms;
- Medical oncologists. A medical oncologist specialises in treating pancreatic cancer with chemotherapy, immunotherapy and targeted therapy;
- Surgical oncologists, who will be able to surgically operate on pancreatic cancer;
- Radiation oncologists can treat pancreatic cancer with radiation therapy.