Lumbar discectomy
Mr Khalid Salem - Orthopaedic surgery
Created on: 11-13-2012
Updated on: 07-24-2023
Edited by: Conor Lynch
What is a lumbar discectomy?
Lumbar discectomy is a surgery that is performed when the patient has a herniated disc in the lumbar part of the spine. This causes back pain that spreads to the legs and causes severe muscle weakness. The surgical procedure can remove part or all of this pad to relieve the pain. A lumbar discectomy is typically done as a minimally invasive (keyhole) procedure.
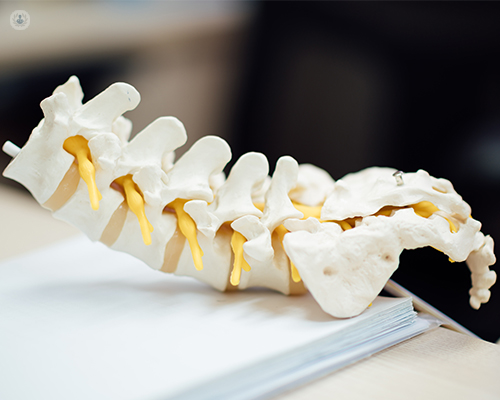
Why is a lumbar discectomy needed?
When a patient has a herniated disc in the lumbar part of the spine. This can also be referred to as a slipped disc, ruptured disc, bulging disc, or a disc prolapse. A doctor will normally recommend having the procedure when the herniated disc is causing:
- trouble standing or walking due to nerve weakness
- physical therapy, steroid injections, and other conservative therapies don't improve symptoms after six to 12 weeks
- pain within arms, legs, buttocks, and/or chest becomes too severe to manage
Possible causes of disc herniation can include:
- gradual degeneration of wear and tear
- a strain or twist
- falling on the back
- a hit or blow in the back
- traumatic events, i.e. a car accident
How is a lumbar discectomy procedure done?
A lumbar discectomy procedure usually takes up to one hour and is done using minimally invasive (keyhole surgery) techniques. The procedure may be done using a local anaesthetic, but some patients may use general anaesthesia.
A small incision will be made on the back at the same level as the herniated disc. During the procedure, a live x-ray may be used to ensure the correct location of the affected disc. Depending on the location, some small fragments of bone and ligament may be removed to gain access.
The doctor will ideally only remove the part of the disc that is pinching the nerve or causing pain. However, sometimes the whole disc needs to be removed. In these cases, possible substitutes to replace it can be: a disc taken from a deceased donor; bone from the patient's pelvis; or a synthetic bone substitute, possibly made from metal, polymers, or ceramic. Afterwards, the adjoining vertebrae will be fused together with metal hardware. The incision wound will be closed and a small bandage will be placed to cover it.
What are possible risks, complications, and side effects?
As with every surgery, there may be some risks and complications. These can include:
- bleeding
- infection
- leaking spinal fluid
- blood clots
- injury to nearby nerves
- allergic reaction to anaesthetic agents
- injury to nearby blood vessels
- brief relief of symptoms, recurrent or continuing symptoms
- paralysis
- deep vein thrombosis
- facial sores and loss of vision, due to position during procedure
- dural tear
What can you expect after the procedure?
As a lumbar discectomy is normally done as an outpatient procedure, the patient will spend some time in a recovery area until they are ready to go home the same day. However, if you have any pre-existing medical conditions, an overnight hospital stay may be required.
Depending on the patient's daily activity and/or how much activity is involved in their work, the doctor will recommend the recovery time. If it is very little, the patient may be able to return to easy lifting, walking, and sitting within two to six weeks. If more activity is required, then it can be six to eight weeks. Check with your physician about the recommended recovery time after the procedure.
There might be some drainage from the incision site, but this is normal. If it feels like an abnormally large amount, notify your doctor. If there are any other serious symptoms, such as a high fever, seek a medical professional.
What is the success rate of a lumbar discectomy?
Some research has shown that a lumbar discectomy is successful 70 to 90 per cent of the time. The results are best in people who show clear signs of nerve compression. Although, as the procedure doesn't do anything to reverse what caused the herniated disc in the first place, it may not be a permanent cure. Success results vary from patient to patient, so you should speak with your doctor to see if it is the best option.





