Autoimmune diseases
What are autoimmune diseases?
Autoimmune diseases are a group of conditions where healthy cells in the body are mistakenly attacked by the immune system.
There are more than 80 different types of autoimmune diseases that affect any part of the body. This makes diagnosis difficult. The most common autoimmune diseases are:
- Inflammatory bowel disease, which includes Crohn's disease and ulcerative colitis. It is linked to a microbe that activates the body’s defence mechanism, causing inflammation.
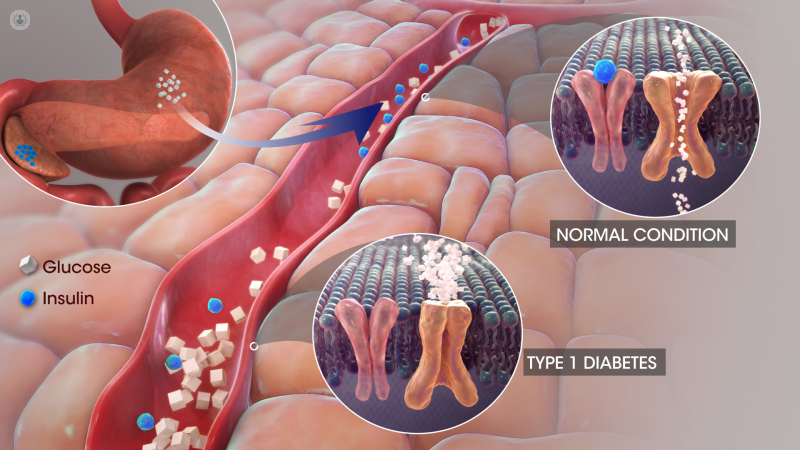
- Type 1 diabetes: the defence mechanisms attack the cells in the pancreas that produce insulin (insulin enables the body to use the glucose it receives). This form of diabetes usually occurs during childhood or adolescence.
- Rheumatoid arthritis: a form of arthritis that affects the joints.
- Multiple sclerosis: a central nervous condition that damages nerve fibres and the protective coating around them (called the myelin). This disrupts the messages travelling along the nerve fibres.
- Coeliac disease: affects the small intestine. The immune system of a person with coeliac disease reacts to gluten, which damages the lining of the intestine.
- Lupus: this can affect any organ, the most common being the skin and joints.
- Other, less frequent, autoimmune diseases include some thyroid disorders, pernicious anaemia, Addison's disease and vitiligo.
Does having an autoimmune disease affect my life expectancy?
Although autoimmune diseases can’t yet be cured and most of these conditions are chronic, there are a number of treatments available which can help alleviate the symptoms. Having an autoimmune disease does not affect your life expectancy and many people with autoimmune diseases will be able to have a normal life.
Symptoms of autoimmune diseases
Despite the different types of autoimmune diseases, many of them share similar symptoms.
The main ones are usually inflammation (which can cause redness, heat, pain and swelling), fatigue, muscle ache, nausea, headaches and fever, but these symptoms do not apply to all autoimmune diseases (particularly Type 1 diabetes).
Symptoms also depend on the particular condition:
- Inflammatory bowel disease: abdominal pain and bloody diarrhoea are common.
- Type I diabetes: blurred vision, the need to urinate often, problems with concentration, and chronic thirst.
- Rheumatoid arthritis: the main symptoms are mild joint pain, stiffness, and fatigue. The joints may be hot and painful. The areas most affected are the wrists, knees, fingers, and ankles.
- Multiple sclerosis: causes numbness, paralysis and vision impairment, depending on which part of the nervous system is affected.
- Coeliac disease: manifests as abdominal pain, diarrhoea, constipation, weight loss, and fatigue.
- Lupus: this may be difficult to diagnose since it manifests as outbreaks. Symptoms depend on each case, but the main symptoms are muscle and joint pain and hair loss. In addition, there is often atypical colouring on the face, especially on the nose and cheeks.
Autoimmune symptoms may vary, from mild in some people to seriously debilitating in others depending on which part of the area is affected and to what degree. Symptoms can also be caused by other conditions.
Medical tests for autoimmune diseases
The first step in detecting an autoimmune disease is to have a complete medical history taken, including family history, lifestyle, drugs prescribed, and symptoms. After this, depending on the autoimmune disease detected or suspected, some tests will be performed:
- Inflammatory bowel disease: may require blood and stool analysis, endoscopy, capsule endoscope, ultrasound and radiological tests.
- Type 1 diabetes: a glycosylated haemoglobin (A1c) test, a random blood sugar test or a fasting blood sugar test is usually done for diagnosis.
- Rheumatoid arthritis: a blood test and radiology examination of the most affected skeletal segments most affected is performed.
- Multiple sclerosis: no single test can positively confirm multiple sclerosis. If there's evidence of at least two separate attacks with multiple sclerosis symptoms, a neurologist may order a neurological examination, an MRI scan, an evoked potential test, a lumbar puncture and several blood tests to diagnose the condition.
- Coeliac disease: four tests are usually performed to diagnose this condition: serology, genetic testing, duodenal biopsy and dietary testing.
- Lupus: diagnosis of lupus is often complicated. Diagnosis is based on the presence of several criteria that must occur at the same time, such as malar rash, arthritis, blood or neurological disorders, mouth sores and serositis, among others.
What causes autoimmune diseases?
The causes of autoimmune diseases are unknown, although they tend to be hereditary. In addition, some viruses, bacteria and drugs may cause certain alterations that trigger their appearance. Smoking, obesity and some medications also increase the risk for autoimmune diseases.
People with one autoimmune disease are often prone to develop another autoimmune disease as well.
Can they be prevented?
There is currently no known way to prevent autoimmune diseases.
Treatments for autoimmune diseases
There are different treatments depending on the disease to be treated. For example, the main treatment for type 1 diabetes is the daily administration of insulin. Patients with coeliac disease need to eliminate gluten from their diet. Patients with rheumatoid arthritis can take anti-inflammatory medication and steroid injections to manage pain. Other treatments include immunosuppressant medication and physical therapy, if mobility is affected.
Do autoimmune diseases make you more susceptible to COVID-19?
People with autoimmune diseases are not more susceptible to COVID-19.
However, some autoimmune diseases, like type 1 diabetes, and certain immunosuppressant medication can increase the risk of developing serious illness from COVID-19. This is because the SARS-CoV-2 virus causes extreme infection and inflammation, putting more stress on the body of people with autoimmune diseases. The ability to fight an infection like COVID-19 is reduced, increasing the risk for serious illness. People with autoimmune diseases should not stop taking their regular medication. If in doubt, patients should speak with their doctor to assess their risk of COVID-19.
As of yet, there is no evidence that suggests that COVID-19 can cause autoimmune diseases.
Which autoimmune diseases are immunocompromised?
People with autoimmune diseases aren't technically considered immunocompromised, regardless of the type of disease, unless they take immunosuppressant medication that dampens their immune system, making them more prone to infections and increasing their risk of illness.
Should I boost my immune system if I have an autoimmune disease?
Boosting or strengthening the immune system isn't particularly desirable, given that the immune system is not a single entity, but rather a system that needs balance and harmony to function well.
People with autoimmune diseases, especially, should not boost their immune system. This is because autoimmune diseases are prone to occur when the immune system overreacts or is overstimulated, causing it to attack healthy cells in the body.
Can autoimmune diseases cause weight gain?
People with autoimmune diseases are susceptible to drastic fluctuations in weight due to inflammation and medication taken. Depending on the condition, this can either be weight gain or weight loss.
Why can't autoimmune diseases be cured?
The immune system is very complex and although there have been advances in research, it is still widely unclear how and why autoimmune diseases develop. This lack of information slows down the development of a cure and the development of effective preventive measures.
Why are autoimmune diseases on the rise?
Scientists believe that this rise can be due to environmental and lifestyle changes (such as eating a low-nutrient diet), which in turn, cause changes in our bodies and in our immune system's ability to respond to infections.
Despite this, genetics and other individual factors, continue to be the leading cause for the development of autoimmune diseases.
Are you born with autoimmune diseases?
If there is a family history of an autoimmune disease, certain genes - which predispose someone to autoimmune diseases - may be present at birth. This can lead to some autoimmune diseases being diagnosed at or shortly after birth. Others may not show symptoms and diagnosis is made later in childhood or in adulthood.
Which specialist treats autoimmune diseases?
The specialist treating an autoimmune disease will depend on the type of disease. Some specialists include: immunologists, dermatologists and rheumatologists.