How common is endometriosis in women?
Written by:Endometriosis is a rarely discussed condition but it is estimated to be present in 35% of all cases of infertility in women. We asked consultant gynaecologist Mr Christian Barnick for an explanation of what it is, who it affects, what symptoms to look out for, what problems it may cause and how it is diagnosed.

What is endometriosis?
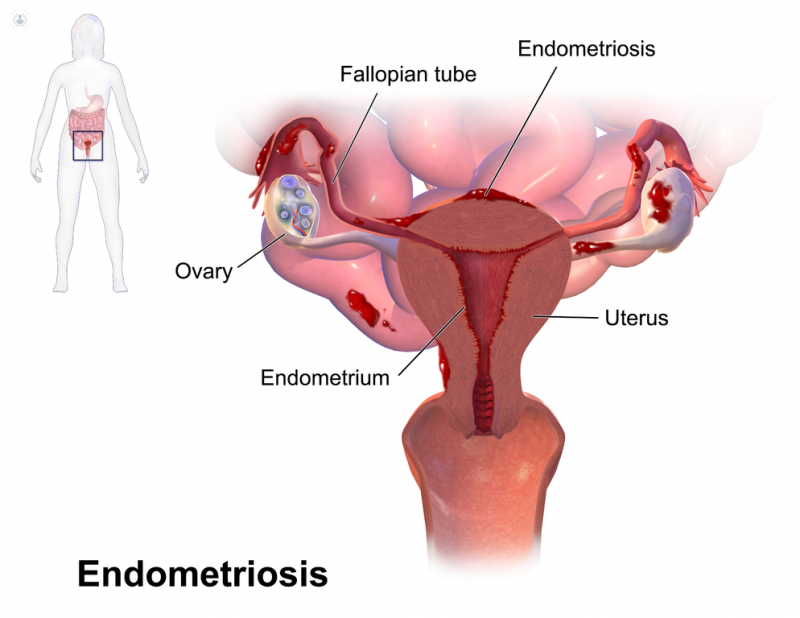
Endometriosis is a benign (non-cancerous) condition where tissue similar to the lining of the womb (endometrium) is found elsewhere in the body, usually the pelvis. Deposits of the tissue might form in the ovaries, on the bladder, or on the large intestine. Each month this tissue bleeds leading to inflammation, pain and the formation of scar tissue or adhesions.
Who does it affect?
Endometriosis is very common, affecting between 10% and 25% of young women. It also appears to be present in 35% of women who have problems with infertility. We are not sure exactly how many women it affects, because it is possible to have the condition without noticing any symptoms, so often it can go undiagnosed.
There is a genetic component to endometriosis, because women are much more likely to develop the condition if they have a mother or sister who suffers from it. Women who take the combined oral contraceptive pill are less likely to develop the condition, and it disappears in women who have been through the menopause unless they are on HRT (hormone replacement therapy).
What symptoms does it cause?
Symptoms of endometriosis can include:
- pain before or during your period
- pain in the pelvis and thighs
- pain during sex
- pain when going to the toilet
- difficulty getting pregnant
The amount of pain women experience does not always correspond to the amount of endometriosis present. Some women, even those with severe endometriosis do not experience any symptoms at all.
What causes endometriosis?
We are not quite sure but we have a few theories. In most women it is likely to be due to:
- Retrograde menstruation – this is where some of your menstrual blood flows backwards into the pelvis and any live endometrial tissue within it may implant and thrive in response to your hormones.
- Endometrial tissue can also spread into the pelvis via blood vessels, lymphatic channels or may implant in surgical scars.
It has been hypothesised that the immune system is normally responsible for preventing endometrial tissue form implanting itself, so the development of endometriosis may be a result of some form of immune disorder.
How is it diagnosed?
When you visit the doctor they will ask you for a history of your symptoms, including which situations cause you to feel pain. Endometriosis symptoms are typically increased pain around the time of periods, radiating down into the legs, up into the loin. Pain during sex is also very common. In most cases, you will have a vaginal examination to see if any endometriosis can be felt.
The doctor might then recommend a vaginal ultrasound, which is particularly good at diagnosing endometriotic cysts (chocolate cysts). This method is excellent, but, depends much on the experience of the ultrasound scanner. If nothing is revealed on the ultrasound, or if the finds are complex then an MRI may be better. Neither of these techniques will pick up small areas of superficial endometriosis and the most definitive diagnostic procedure is still laparoscopy.
This involves inserting a telescope, through the belly button, under general anaesthetic. This allows the surgeon to carefully inspect all of the abdominal cavity. If any endometriosis is found then the surgeon should aim to excise it at the time, without removing the womb or damaging the ovaries or fallopian tubes.


