Gastrointestinal endoscopy
Dr Ian Arnott - Gastroenterology
Created on: 11-13-2012
Updated on: 04-20-2023
Edited by: Carlota Pano
What is a gastrointestinal endoscopy?
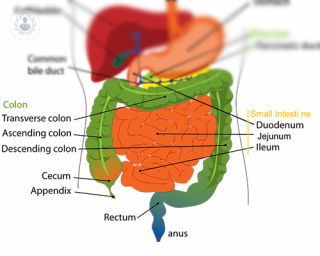
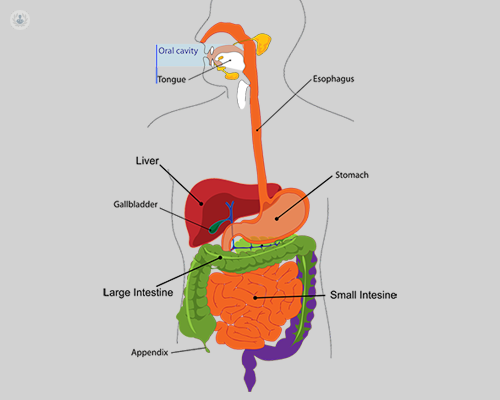
A gastrointestinal endoscopy, also known as gastroscopy or digestive endoscopy, is a test that is used to diagnose and treat diseases of the upper digestive system. The upper digestive system comprises of the oesophagus, the stomach and the duodenum (the first part of the small intestine).
What does it consist of?
An gastrointestinal endoscopy is carried out with a tool called an endoscope. This is a thin and flexible tube with a camera, and sometimes a light, at the end. The endoscope is inserted through the mouth and the images captured are displayed on the monitor in real-time as the endoscope advances in the body and/or recorded.
Other tools can be placed inside the endoscope. This means that specialists can perform other tests (such as a biopsy) or perform treatments (such as the removal of polyps and cauterization of bleeding blood vessels) at the same time.
The procedure lasts around 15 to 30 minutes. However, in the event that something unexpected is found, or a quick treatment or biopsy has to be taken, it can last longer.
Why is a gastrointestinal endoscopy performed?
There are several reasons why a digestive endoscopy may be performed:
- Analyse oesophageal problems such as esophagitis, a narrowing of the oesophagus or tumours
- Analyse stomach problems: gastritis, tumours and stomach ulcers
- Diagnose a hiatal hernia and/or gastroesophageal reflux disease (GERD)
- Detect liver cirrhosis - in these cases there may be thickening of the stomach and oesophageal veins
- Assist in discovering the cause of hematemesis (vomiting blood)
- Assist in diagnosing the cause of anaemia – a loss of blood in the digestive tract can result in a lack of iron
- Gather samples for diagnosing coeliac disease or bacterial infections
Aside from being used as a diagnostic tool, digestive endoscopies can be used for other purposes:
- Remove foreign bodies that could have remained in the upper intestine
- Dilate the oesophagus if it has become narrowed
- Remove polyps from the intestine
- Cauterize bleeding vessels (stop blood flow)
- Ligating oesophageal varices that may bleed
Preparation for a digestive endoscopy
Consumption of food or drink should be avoided in the eight hours prior to the procedure. Also, some patients may be told by their specialist to stop taking their regular medication.
The patient won’t be given any medication before the procedure. However, sometimes a local anaesthetic may be applied to the throat to reduce possible nausea.
Occasionally, intravenous sedation will be administered to relax the patient.
What do you feel during the exam?
Gastrointestinal endoscopy is a painless procedure and can sometimes only last between three and five minutes. Despite not being painful, it is likely that the patient will notice some discomfort and may feel constant nausea while the endoscope is inserted.
Once the examination is finished, the patient will feel discomfort and numbness in their throat. They may feel like they have excess gas due to ingested air, but this will disappear quickly.
Meaning of abnormal results
The digestive endoscopy procedure is quite a safe test and complications appear scarcely. The possibility of complications increases the moment the endoscope is used to perform a type of treatment.
Possible complications are:
- Perforation
- Reaction to medication
- Haemorrhages (bleeding)
- Cardiopulmonary alterations
Advances in endoscopy
Thanks to endoscopies, problems that previously required surgical intervention can be diagnosed and treated without it.
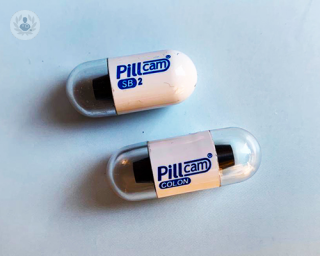
In parts of the digestive tract where the gastrointestinal endoscope cannot reach, there is the capsule endoscopy, in which a tiny camera is ingested like a pill. This transmits images of the digestive system to a monitor and leaves the patient without any discomfort.